How has public health mask guidance gotten so out of step with what we know is safe?
Most people now accept that COVID-19 is airborne. For those with lingering doubt, the contagiousness of the Omicron variant is now understood to be roughly tied with (or slightly ahead of) the most infectious virus known to humans. That virus is Rubeola, which causes measles, and it is so contagious that a person can readily infect an entire room of people — even if patient zero leaves well before the others arrive. Efficient airborne transmission is the only conceivable way for Omicron to spread so aggressively. As a result, here is what all of us should do...
Get and wear a properly fitting N95 mask.
Expert consensus is that the appropriate and effective mask technology for airborne contagion is a properly worn N95 (or one of its common variants, CN95, FN95, KN95). Yet, in the fight against COVID-19, community use of N95 masks has not been encouraged by governments or public health authorities. Instead, guidelines for the public usually prescribe a homemade cloth mask, or a blue rectangular medical mask, to prevent transmission at close range by large droplets.
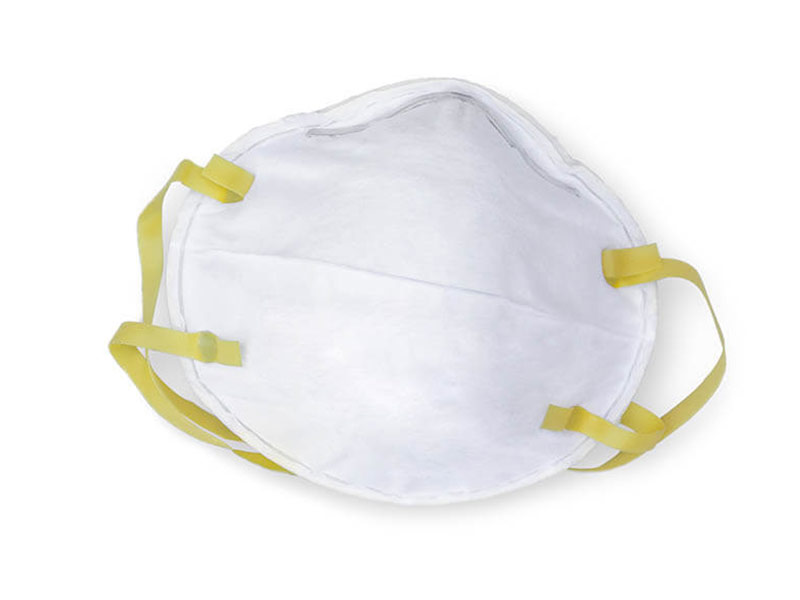
It may seem puzzling that N95 masks are not heavily promoted to protect against COVID-19 exposure. There should be no doubt they are superior. The fabric used in an N95 mask is certified to filter out 95 per cent of tiny contaminating particles from the air, providing excellent (not perfect) protection. However, what is truly vital is its particular capacity for snug fit: any mask is ineffective when air is inhaled and exhaled around it rather than through it.
However, some do insist that all types of mask provide similar protection for the wearer. This view is based on lab studies showing that under perfect conditions, high-quality medical masks and high-quality three-layer cloth masks have excellent filtration capability. But daily life does not unfold under perfect conditions, which is why so many blue medical masks and cloth masks make visible so many nostrils. By contrast, a properly donned N95 mask tends to stay put, maintaining an excellent fit to enable its excellent filtration.
Wear an N95 mask when indoors with others beyond your household circle.
Logically, during a pandemic of a highly contagious airborne virus, an N95 mask should be worn when people are compelled to share indoor air in the course of daily activities. This is even more important in the company of particularly vulnerable groups, such as the elderly, or children too young to be vaccinated.
Yet paradoxically, resistance to N95 masks sometimes appears even in higher-risk settings. For example, many school boards in Ontario actively forbade teachers from bringing their own N95s to work, insisting on the standard-issue medical mask, under threat of discipline. Visitors to hospitals have frequently found themselves compelled to exchange their N95 mask for an ill-fitting blue one. Barbers in Toronto were directed by local public health to replace their cloth mask or N95 mask with a baggy blue rectangle. Tellingly, while Health Canada’s website does quietly acknowledge community use of N95 masks, there are no public service messages to guide people how to find, fit and wear one.
Understand the flaws in logic that discourage N95 mask use.
How did we get to this dangerous state of affairs where medical or cloth masks, suitable for droplet transmission with their gaps at the top and sides, are favoured over N95 masks? The cause is not hard to find. The seat of expertise in PPE lies with Infection Prevention and Control units in our hospitals. Their strict protocols govern the use of PPE in acute settings, and also elsewhere by default. Unfortunately, these protocols are predicated on two gaping logical flaws. Tragically, the harm from these flaws is far-reaching; because IPAC units claim a monopoly on infection prevention expertise, they control the PPE discourse for everybody, including those who work in government and public health.
The first IPAC logic flaw is to follow relentlessly its own published protocols, despite urgent, emerging evidence to the contrary. These protocols baldly proclaim large-droplet transmission for respiratory viruses; this has been the prevailing belief for decades, and evidence-based protocols take many years to evolve. The protocols dictate that N95 masks are only for airborne pathogens, therefore not suitable for COVID-19. Public health leaders who recite the litany of physical distancing, plexiglass, hand hygiene and medical masks are toeing this line. One particularly perverse application of this logic saw IPAC audit teams actually entering long-term care homes in Ontario to remove N95 masks from hapless personal support workers caring for COVID-positive residents.
However, many health-care workers do wear N95 masks when caring closely for COVID patients in hospitals. In this inconsistency lies the second dangerous flaw in IPAC logic: the supremacy of the N95 “fit test.” Health-care workers caring for highly contagious patients in an isolation room must undergo N95 fit test certification to establish that a specific brand and shape of N95 mask can form a perfect seal for a specific person: not every mask will perfectly fit every face shape, so a fit test has great value in making this determination. However, by unthinking extension of IPAC logic, activities such as grocery shopping are held to the same exacting standard as entering an active isolation room. And because regular people do not have access to fit test certification, IPAC protocols forbid them from wearing an N95 mask at all. This faulty reasoning is based on the supposition that nobody can be trusted to learn how to wear an N95 mask that fits them any better than a loose blue rectangle. Some face shapes do happen to be fairly compatible with a medical mask, but that is cold comfort for everybody else.
Help each other find N95 mask sources, given the limited supply.
One consequence of limited demand is limited supply. By governments continually signalling to industry that N95 masks are for limited use only, neither investors nor manufacturers have had good reason to scale their production to anything near what we urgently need, not in Canada or elsewhere. This is particularly unfortunate because the 18-month period since airborne transmission began to be evident was ample time to grow capacity, here and abroad. The logic of limiting community N95 mask use for an airborne virus would seem to be a global folly. Given current shortages, the use of an elastic “mask brace” to help press the edges of a medical mask to the face may be of practical use to many, but it is far from ideal.
Help get the word out on N95 masks.
A failure to promote N95 masks is dangerous public health misdirection. We trust people to determine which shoes, hats and diapers fit well without a certification test. We should promote the same personal agency for N95 masks too. This will soon begin happening in Ontario, with N95 masks recently promised to teachers. But more needs to be done. Public service messages need to provide easy tips to help enable a good N95 fit, miles safer than the blue rectangle for most people. Public health authorities ought to be distributing sample packs with several different mask designs, to let people easily find the fit they need in order to be safer in class, on the bus, or at the mall. Governments could and should be making N95 masks freely available: by any measure they are less costly than looming lockdowns.
We urgently need to reject the rote application of IPAC logic in community settings. In its place, we need new policy for community PPE to enable people to work, study, shop and travel safely. Such policy would be usefully informed by IPAC experts, but it should not be led by them. At least not for the years it may take for their protocols to catch up to what we know. ![]()
Read more: Coronavirus
















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: