In 1889, a mysterious disease arose in the Asian city of Bukhara, an ancient trade centre in what is now called Uzbekistan. It soon spread to the port city of St. Petersburg in Russia. By December it had conquered most of Europe, catching free rides on newly completed continental railroads or shiny steamships that crossed the Atlantic in six days.
Everyone called the malady the Russian flu or that “dreaded Russian disease” because it travelled from the East with a rapidity that would not have surprised Omicron observers.
At the time, physicians initially discounted the outbreak as nothing more than a "jolly rant" or another cold. Most predicted a mild and short visitation. They were wrong on both points.
The “dreaded Russian disease” persisted in waves over a five-year period, eventually killing more than 1.5 million people on a planet then inhabited by only 1.5 billion humans. It reappeared in 1900.
About one in 100 people infected by the contagion either died from pneumonia or experienced severe illness affecting the brain, lungs or stomach. The breadth and persistence of the outbreak reintroduced the word “pandemic” to the English vocabulary.
To this day, the little-known biological storm ranks as one of the globe’s great disease outbreaks in terms of scale and mortality.
Now, 133 years after that event, virologists and historians suspect that a novel coronavirus triggered the so-called “Russian flu pandemic.” Many view this pandemic as a dramatic historical preview of the current one — complete with variants, waves and longhaulers suffering from chronic neurological complications.
Here are five scenes from this fascinating and evolving story:
After Severe Acute Respiratory Syndrome, or SARS, scared the world with an aborted outbreak that killed 800, the coronavirus family suddenly fell into scientific fashion.
In particular, many researchers wondered about four members of this virus family — types 229E, NL63, OC43 and HKU1 — that cause common human colds. Were they as benign as they appeared and did they begin their evolutionary careers that way?
A group of Belgian scientists at the Leuven University began that inquiry by sequencing the genome for OC43. To their surprise, it bore many genetic similarities to a disease-causing coronavirus in cattle. (Most coronaviruses live in animals — everything from whales to bats.)
First identified in 1967, OC43 accounts for about 10 to 30 per cent of all the sniffles and other minor ailments people associate with having “a cold.” As a consequence, medical authorities gave it short shrift.
In contrast, when veterinarians discovered a bovine coronavirus in Nebraska in 1971, they took a different attitude. The bovine coronavirus not only caused severe diarrhea in calves, but it was later found to cause winter dysentery in adult cows and shipping fever in feedlot cattle. Researchers eventually called the triumvirate illness — needing several factors to elicit sickness — Bovine Respiratory Disease Complex, or BRDC. Researchers suspected that the emergence and spread of BRDC had a lot to do with “existing herd management practices including crowded housing, transportation, constant influx of new animals, production-associated stresses in cows.”
Puzzled by similarities between BRDC and OC43, the Belgium researchers performed what is called “a molecular clock analysis” and traced the evolution of the two viruses back in time to approximately 1890. That’s where they found a common ancestor in cattle for both viruses.
Around 1890, the bovine coronavirus diverged and popped into human populations as OC43, where it began another evolutionary journey that ended unpredictably as a common cold.
The researchers cited some striking arguments to support their hypothesis. In the second half of the 19th century, a number of highly infectious epidemics or murrains plagued cattle around the world as urbanization, globalization and industrialization unsettled agricultural landscapes. They included a mycoplasma, rinderpest and possibly coronaviruses — long a fixture of wild ruminants.
The outbreaks prompted massive killings of infected cattle. The relentless culling created opportunities for the spread of animal viruses from their handlers to urban populations and other ruminants as well.
In addition, the researchers noted that a troubling influenza pandemic had swept over the world in 1890. The symptoms of the pandemic included high fever, pneumonia and strange central nervous system disorders that often lasted for years. What’s more, influenza viral experts had not been able to trace the pandemic to a particular influenza subtype with any real precision.
The study concluded that the SARS outbreak in 2003 wasn’t an anomaly, but part of a phenomenon that proved the “viral promiscuity” of coronaviruses. The study appeared in the Journal of Virology with little fanfare and was largely forgotten until the 2019 pandemic.
Dr. Henry Franklin Parsons, a distinguished physician in England, had a problem. Alarmed by a troubling influenza epidemic that had given “rise to much inconvenience” and “much pain,” the British government had asked him to file an extensive report.
But Parsons faced a medical puzzle. Although the epidemic definitely appeared to be some form of influenza, it didn’t exactly behave that way.
“The catarrhal symptoms have been less recent than in many former epidemics,” noted Parsons in his 1891 Report on the Influenza Epidemic of 1889-90.
The general absence of congested nasal passages and sniffling in so many of the sick led some observers “to doubt whether the recent epidemic has been one of true influenza,” wrote Parsons.
One chronicler bluntly described some of the afflicted as “persons in a peculiar dazed stupid condition for about two weeks, unable to think or do their work.”
In addition, the strange malady primarily struck down older adults and left children relatively unscathed, which wasn’t how classic influenza normally worked.
Persons with weak lungs and those suffering from heart disease or kidney troubles also appeared to be most seriously affected. Death by pneumonia was not uncommon.
Other doctors told Parsons that they likened the outbreak not to influenza, but to malaria and dengue fever. They noted that the dreaded Russian disease caused “distressing pain” in the forehead, temple, eyes and face. Some even prescribed quinine, an anti-malarial drug, for treatment.
Moreover, these neurological pains reoccurred in devastating bouts. The infected also lost their sense of smell and taste.
In the end, Parsons carefully catalogued all of these puzzles, but stuck to his influenza diagnosis. He explained away the anomalies by noting many physicians really hadn’t seen an influenza epidemic before (the last one to hit England occurred in 1847) and that maybe the weather accounted for some of the different symptoms.
But Parsons wasn’t the only doctor to note a raft of inconsistencies. In Ontario, Canada, the Hamilton Herald reported that the Russian flu “differs entirely from any previous kind of influenza,” adding that “it visits the seat of disease which is incident to the person attacked such as the kidneys, liver, lungs and heart.”
As medical historian and journalist Mark Honigsbaum started hearing more stories about the baffling conditions experienced by COVID-19 longhaulers, he realized that historically, they weren’t alone. Nor were they the first.
Like COVID, the Russian flu left behind a large population of invalids suffering from a bewildering array of neurological symptoms, including loss of memory, loss of energy, anxiety and “post-grippal numbness.” The conditions, which often lasted years, intrigued and baffled doctors throughout the 1890s.
As Honigsbaum noted in an article in The Lancet: “The official end of the pandemic, therefore, did not mean the end of illness but was merely the prelude to a longue durée of baffling sequelae.”
One specialist doctor even observed the dreaded Russian disease “runs up and down the nervous keyboard stirring up disorder and pain in different parts of the body with what almost seems malicious caprice.”
The English suffragette Josephine Butler, for example, compared her chronic ailment to a bout of malaria.
“I am so weak that if I read or write for half an hour I become so tired and faint that I have to lie down,” Butler wrote to a friend.
Other public figures felled by insomnia and fatigue included the British prime minister and even the First Lord of the Admiralty.
Long-term complications from the Russian influenza were so prevalent, that by the middle of the 1890s, doctors blamed everything from rising suicide rates, to general feelings of unease and depression to the long shadow of the disease. In fact the pandemic’s invalids became “central to the period's medical and cultural iconography,” noted Honigsbaum.
But unlike the current pandemic, sufferers of long-term symptoms received unparalleled attention from the medical community throughout the 1890s. With fewer experts, general practitioners paid more attention to the whole patient and wrote entire treatises on the flu’s longhaulers.
Honigsbaum then offered some advice to the current medical community, which has been slow to recognize the scale and significance of long COVID: “As they adjust to the pandemic's longue durée, physicians might find it helpful to look back to the Russian influenza and the historical accounts of the sequelae, even as COVID-19 longhaulers look to digital, patient-centred and activist forums for support and validation in the present.”
A year later, Honigsbaum wrote that if the Russian flu pandemic was indeed due to a coronavirus that infected at least 60 per cent of the population, the experience does not auger well for the future.
“Herd immunity does not appear to have been reached hence the recurrent waves of illness, marked by high mortality.”
Intrigued by the growing parallels between COVID-19 and the Russian flu pandemic, Harald Brüssow, another researcher at Leuven University, reviewed the medical literature on the 130-year-old outbreak, including Parsons’ report.
He found that Parsons wasn’t the only doctor to notice that the “Russian flu” behaved in weird ways. Or like COVID-19 today.
Clinical data from German medical reports, for example, told a familiar story: “Neuralgic pain and prostration is prominent and for 92 per cent of the patients neurological complaints dominated the disease. Patients noted mostly headache, and less frequent back and muscle ache. A quarter of the patients were incapable of resuming their usual activity even without showing other symptoms of illness.”
The Germans also reported episodes of blood-clotting, just as physicians have with COVID: “Phlebitis and thrombosis was frequently observed in the recovery phase, even deadly cases of sinus thrombosis occurred. Striking were cases of thrombosis in arteries.”
Given that the Russian flu pandemic came in three waves, Brüssow speculated that they “might represent the appearance of variant viruses.”
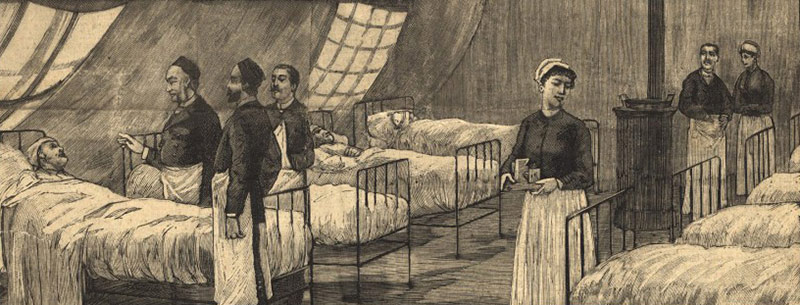
Reports from the 1890s also found crowding and insufficient ventilation led to mass infections. The sick overwhelmed hospitals and the military set up tents for the afflicted. Schools and universities closed. Mortality rates increased by 30 per cent compared to pre-pandemic years in some cities. In Madrid, the authorities ordered funerals to take place at night so as not to alarm the living.
Brüssow also discovered that pandemic apparently re-emerged in 1900, killing a good number of physicians with a multi-organ disease. At the time, doctors tellingly classified this outbreak in The Lancet into four categories: One attacked the mucous membranes; another hit the gastrointestinal tract; a third attacked the heart; and a fourth targeted the nervous system. Patients suffered from shortness of breath, thrombi in the brain, loss of smell and even developed diabetes after being infected.
The researcher offered a brief conclusion: “Since these observations resemble more of a COVID‐19 related disease than classical influenza, we must consider the possibility of a coronavirus‐induced pandemic in 1889–1890 and a resurgence of this pandemic 10 years later, peaking in 1900.”
In a separate paper, Brüssow asked what the 1890 pandemic might tell us about the unpredictable progress of COVID.
Given a divided global population of eight billion people armed unequally with a variety of medical interventions, “it is by no means clear whether an epidemic with similar base characteristics will be a replay of one which occurred 130 years ago,” he wrote.
He added this sobering thought: “If the data from the end of the 19th century are an indication, COVID-19 may occupy us for a decade in multiple infection waves without much clinical attenuation if not stopped by vaccination programs that achieve herd immunity or breakthroughs in drug development which make COVID-19 a treatable disease with low mortality.”
Convinced that coronaviruses have probably played a critical role in previous epidemics, a team of researchers from Arizona and Australia parsed the human genome for evidence.
About 20,000 years ago, a coronavirus epidemic left an imprint on the DNA of people living today. The outbreak interacted with human genes in East Asia and left behind a calling card: antiviral modifications in at least 10 different human genes.
The gene fortification only occurred in an East Asian population and probably required a lot of deaths for the human genome to respond with these modifications.
The researchers concluded that ancient RNA virus epidemics have probably occurred frequently in human evolution.
“It should make us worry,” David Enard, an evolutionary biologist at the University of Arizona, told the New York Times. “What is going on right now might be going on for generations and generations.” ![]()
Read more: Coronavirus

















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: