“Today is a day to remember and grieve. And also a time to act.” So pronounced Jason Luan, Alberta’s associate minister of mental health and addictions, in a statement to commemorate International Overdose Awareness Day. The date was Aug. 31. A hot spell was tailing off in the windswept prairie town of Lethbridge, offering the slight first hint of autumn’s chill.
Overdoses are preventable, Luan emphasized in his public letter. “Everyone deserves to have the opportunity to recover from addiction.”
That same day, Lethbridge’s only supervised drug consumption site — believed to be the busiest in North America — shut down after Luan’s ministry pulled funding. It made the decision after an audit of ARCHES, the non-profit that ran the facility, uncovered significant financial mismanagement.
If the organization’s dollars didn’t add up, a different set of numbers signalled its own alarm. Frontline workers in Alberta had been dealing with a dramatic spike in opioid-related deaths during the pandemic. In British Columbia, fatal overdoses had reached record highs.
The ARCHES site, a large, drab building in the city's downtown, opened in early 2018. It was seeing up to 800 visits a day. In its first year and a month, ARCHES employees reversed more than 1,800 overdoses.
Instead of taking over the site, the government replaced it with a converted motorhome. At ARCHES, up to 13 people could inject and eight could inhale substances at one time. The mobile replacement can only hold three people and only those who want to inject.
For Tim Slaney, Aug. 31 marked his last day on the job at ARCHES. A former IV drug user himself, Slaney had worn multiple hats as outreach worker, drug checker, overdose responder. As he said goodbye to one client, he wondered, “What are the chances that this is the last time I see him because no one's going to be there when he goes down?”
In the afternoon, Slaney walked a few blocks to Galt Gardens, the park at the epicentre of Lethbridge’s overdose crisis. There a couple of private security guards asked Slaney for naloxone, an emergency medication that can reverse an overdose. The guards were already witnessing a couple of ODs a day, they told him. Slaney gave them what he could. The guards looked like they had just graduated high school, he remembers. “They were scared, I guess.”
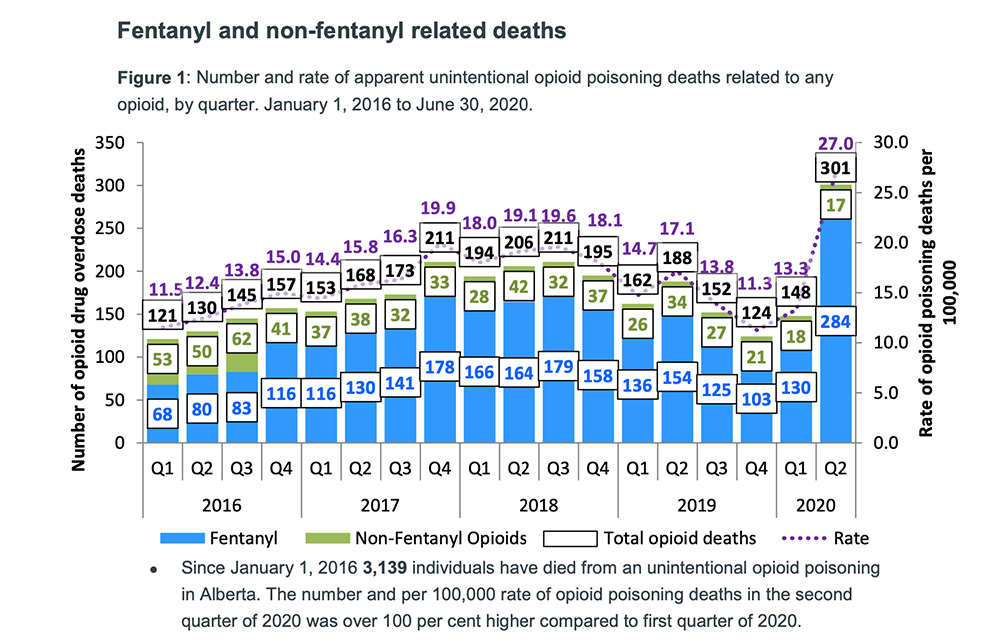
A few weeks after ARCHES closed, the province released its latest opioid overdose numbers. Three-hundred and one Albertans died between April and June — more than three deaths a day — by far the highest quarter on record. One likely reason for the sharp rise, said the report, were barriers to safe consumption sites, leaving more people to use alone.
Another revelation: Lethbridge has experienced the highest rate of fentanyl-related overdose deaths in all of Alberta this year — double Calgary’s rate.
So why hadn’t the government just taken over operations at ARCHES site instead of killing it, wondered Slaney along with other harm reduction advocates. “I’m tired of attending vigils. I’m tired of finding out that someone died. I’m tired of reading obituaries,” he said to himself.
He decided to enlist in the grassroots fight against overdose deaths. Add Tim Slaney to the growing ranks of Alberta’s harm reduction volunteer army.
In the tent
On nights when the Chinook winds don’t gust too hard, you now can find Slaney in a bright orange tent in the middle of Galt Gardens. This is Alberta’s first unsanctioned overdose prevention site, established on Sept. 25 by Slaney and a few other former ARCHES employees who’ve named themselves the Lethbridge Overdose Prevention Society.
Like a lantern in the darkness, the tent draws people seeking a safe place to use drugs, police officers and angry protesters who want it gone. The night the illegal experiment opened Slaney says four people used substances under supervision. Since then, he says, Lethbridge police have stood in the way by threatening to arrest visitors if they do drugs. Volunteers instead offer new needles, naloxone kits or help accessing detox. Sometimes they hand out snacks or clothing, or simply provide people a place to warm their hands.
Days after the orange tent first appeared, Luan asked police to shut it down. The City of Lethbridge has issued Slaney multiple tickets and court summons for setting up a structure in a park without a permit. Meanwhile, Lethbridge Overdose Prevention Society is preparing to apply for a federal exemption so the site can operate legally. For now, it’s only open Sunday through Tuesday, and most of the time it can’t offer the service it’s set up for.
The Lethbridge Police Service neither confirmed nor denied that officers had threatened to arrest people if they used drugs inside the tent. They said they were there to keep the peace — a valid concern.
Video footage shows opponents of the pop-up site barraging volunteers with curses and slurs. One spat on a LOPS supporter who had come to drop off food. During a rare moment when police weren’t present, Slaney says, several protesters rushed the tent, snapping pictures and taking videos in an attempt, he believes, to catch someone injecting and report them to police. They weren’t successful.


Protester Sarah Villebrun says she comes by LOPS to livestream the scene on Facebook. A park frequented by families is not an appropriate place, she says, for an “injection tent.” Exposure to drug use could traumatize children, she argues. Opponents have also claimed that LOPS is made up of outsiders seeking to “destroy” Lethbridge.
Villebrun denied protesters are aggressive or verbally abusive, though she admitted she once attempted to tear down the tent.
Miranda is a 54-year-old grandmother from the local Kainai First Nation who uses a wheelchair to seek support at LOPS. When she has arrived, she says, protesters have called her and other clients dogs and pigs.
Her dependence on opioids started after her doctor prescribed painkillers following back surgery a few years ago. Then he cut her off. Then two of her children, she says, were murdered within a short period of time. She began using street drugs to numb her pain.
Miranda, who did not want to share her last name, told The Tyee she rarely visits Lethbridge’s new mobile service because she feels judged by some of the staff who work there. At ARCHES, she felt like “family.”
“If it wasn’t for ARCHES, and the people that worked there, a lot of us would have given up a long time ago. We relied on that place because we were able to talk to somebody, tell them our problems. They listened to us.”
Besides counselling, she said staff also helped people access resources for the homeless and treatment programs like opioid agonist therapy, which involves pharmaceutical-grade opioids that curb a person’s cravings and reduce withdrawal symptoms.
“I don’t understand why they closed it,” Miranda said through tears.
When Miranda casts her eyes across Galt Gardens, she sees several spots where friends have overdosed and died in the weeks since ARCHES closed. “Sometimes I just feel like letting go,” she says. “I’m tired of seeing all the hurt and pain.”
The rollback
The United Conservative Party’s victory last spring marked a shift in Alberta’s drug policy. Since then, Premier Jason Kenney, a former Harper cabinet minister, has steadily chipped away at harm reduction measures that public health and drug policy experts insist save lives amid an increasingly toxic drug market.
This past summer, an innovative supervised consumption service administered by phone was axed mere hours before its scheduled launch. Next spring, dozens of Albertans with severe opioid dependencies may lose access to a lifesaving treatment called injectable opioid agonist therapy.
Meanwhile, funding for proposed safe consumption sites remains frozen, and Alberta’s existing sites operate in a state of limbo, their short-term funding due to end March 31, 2021. What happens after that is unclear.
“We are taking a city-by-city approach looking at local needs and realities as we determine what’s best moving forward,” Kassandra Kitz, spokesperson for Luan, said over email. “None of these decisions have been made at this point.” Luan declined an interview request.
Kenney, while in opposition, railed against safe consumption sites. As premier, his government released a review of them that focused solely on the disturbance they can cause in their surrounding neighbourhoods. The government had explicitly prevented the review panel from assessing the benefits these services offer people who use drugs, drawing sharp criticism from harm reduction organizations across Canada.
Benjamin Perrin, a former criminal justice advisor to Harper, described the report as a “deeply problematic and biased political document” made up of “cherry-picked” public grievances. Luan called it a “wake-up call.”
As B.C. implements a groundbreaking effort to secure and distribute a safe supply of untainted drugs or alternatives for users, Alberta’s premier has flatly ruled out such an approach. “Free drugs for addicts paid for by taxpayers? It’s a big no,” an incredulous Kenney said in September. His stance ignores the advice of Canada’s top doctor and many other public health experts.
For his part, Luan has questioned the need for what he calls an “unethical” safe supply. In May, he said police in Edmonton and Calgary told him street drugs were no more toxic in 2020 than “in recent years,” despite warnings from public health experts that what’s on the street has become even more toxic due to COVID-19.
Four months later, the province revealed that fentanyl was present in all but six per cent of overdose deaths in Alberta between April and June, the highest share of fentanyl-related deaths in a single quarter.
What, then, is the Kenney government’s answer to Alberta’s overdose crisis? In short: Shift focus away from harm reduction towards treatment and recovery. The UCP government has committed $40 million to battle the opioid crisis. Another $25 million has been earmarked to build five new recovery centres, with a promise to open 4,000 new treatment spaces over the next four years. This substantial investment has won praise from those who run Alberta’s rehab centres, many of whom only offer abstinence-based programs.
“Instead of just telling people where to go and shoot up with poison, how about we open up more detox beds and more treatment centres to show real compassion,” Kenney told the Calgary Sun last year.
To which Petra Schulz responds, “If you let people die, that is not compassionate. That is brutal.” Schulz, a founder of Moms Stop the Harm and one of the government’s most vocal critics, says rehab works for those able to commit to it. In the meantime, she says, “It’s compassionate if you meet people where they’re at, instead of making them arrive at your point, which is what the government is doing.”
Schulz, who lives in Edmonton, lost her son Danny to an accidental overdose in 2014. She says she’s all for treatment and recovery programs, as long as they’re evidence based. But harm reduction must come first.

“We enable people to live, and to have an opportunity to make a change in the future, if the person wants to, and if the time is right for them.”
For some, that’s not realistic, she added. Some are worse off when they stop using. “But as a mom who lost a child, recovery is what we all dream of.”
Toxic words
With the pivot in drug policy by the Kenney government came a sharp change in tone, as well. Under the previous NDP premier Rachel Notley, harm reduction advocates say their input was welcomed and respected. During the NDP’s time in power, Schulz served on a commission to advise the government on its response to the crisis.
But now, a veteran advocate speaks for her colleagues when she says, “our backs are against the wall.” She prefers to remain unnamed given the current climate in Alberta.
The dismissive attitude starts with Kenney and is reflected down the chain. Harm reduction advocates are caricatured by a top Kenney aide as enablers of addiction uninterested in genuinely helping people. Harm reduction itself is a failed experiment — “take a stroll down East Hastings,” says Kenney — despite overwhelming evidence showing it saves lives, including in Vancouver’s Downtown Eastside.
And those who criticize the government, including grieving mothers like Schulz, face online sarcasm from provincial officials. Last year, in response to a tweet by Schulz extolling the health and cost-saving benefits of safe consumption sites, Luan suggested Big Pharma may have bankrolled the research Schulz had referenced. He later deleted the tweet.

According to interviews with numerous people working in harm reduction and drug policy, the government’s hostility to their efforts has cast a pall. Workers at safe consumption sites fear punitive funding cuts if they criticize the government. Mayors don’t want to poke the bear for the same reason. Academics wonder if saying the wrong thing will prevent them from one day securing tenure. Medical workers worry their advocacy could leave them blacklisted by the AHS.
“It’s really unfortunate, because they’re the ones who likely have the some of the best perspectives to bring to the table,” said Corey Ranger, a B.C.-based nurse who previously worked on the frontlines of Alberta’s overdose crisis.
“But they don't know how they can speak out against those injustices,” he says, “because there’s fear of punitive measures, because this is a really vindictive government that would rather engage in ad hominem attacks and gaslight people who speak out against them than actually solve the problems themselves.”
The Alberta government did not respond to The Tyee’s questions about these charges.
Sasha, an Alberta-based academic with a focus on harm reduction methods, requested anonymity for fear of facing professional repercussions, explaining, “There are people who are stepping back from being vocal because they worry that they’ll have a target on their back.”
Like Schulz and other outspoken advocates, Sasha has faced frequent attacks on social media. Once, an angry man left a profane voicemail at their university. “I never received that in the prior government even though I was speaking out just as much,” they say. Sasha is convinced the government’s polarizing approach has fuelled such conflict.
But members of Alberta’s grassroots harm reduction army are not lying down. They’ve created, for example, a Twitter account called the Overdose War Room (a cheeky play on the UCP’s own “energy war room”) where people like Sasha can anonymously vent and rally the troops.
“I don’t feel like I’m gonna shut up,” they say. “There has to be a record of people that objected.” Sasha compares the “stigma and silence” of this moment to the AIDS epidemic of the 1980s.
The lawsuit
In September, a group of 11 patients in Edmonton and Calgary enrolled in injectable opioid agonist therapy launched a lawsuit to stop the Alberta government from ending the treatment they consider lifesaving. The plaintiffs say the government’s decision to pull the plug on the program, which goes by the acronym iOAT, breaches the Canadian Charter of Rights and Freedoms, including the right not to be subjected to any cruel and unusual treatment. Like the unsanctioned OPS in Lethbridge, the group is crowdfunding its legal fight.
One of the plaintiffs is a 29-year-old roofer from Calgary named Dustin Anderson.
Raised by a single mother, Anderson spent much of his childhood homeless before landing in foster care. In his late teens, a car accident left him with a serious injury and a prescription for hydromorphone. He soon became dependent on the painkiller. Like many others across North America, Anderson turned to the street after his doctor stopped prescribing to him and began using oxycodone and other opioids.
For a while, the money he made on the oil rigs in Northern Alberta let him sustain his dependence, as well as keep it hidden. But when Anderson lost his job after the economy crashed in 2009, it took over. He ended up on the street and eventually in jail. Multiple overdoses and a drug-related spinal infection nearly killed him.
Then he found iOAT. “That place saved my life,” Anderson says. He no longer uses street drugs. Instead, he visits an iOAT clinic once every day or two to inject a safe supply of long-lasting hydromorphone. It wards off debilitating withdrawal symptoms, allowing Anderson to maintain his job and “function normally.” Patients in iOAT can visit the clinic for treatment up to three times a day.
The previous NDP government launched iOAT as a pilot project in 2018, opening clinics in Edmonton and Calgary. Kenney’s government renewed the program for one year this past spring. The treatment, which is available in other parts of Canada, is often considered a “last resort” for people with severe opioid use disorder who have failed to respond to other forms of treatment. As of early September, the government said less than 60 people remain in the program. The number of patients in the program once hovered around 100, according to those behind the lawsuit.

According to the lawsuit, some patients have been prematurely transitioned out of iOAT onto a less intensive treatment option “ahead of recognized clinical guidelines” in order to reduce the number of patients as the program winds down.
Beyond the struggle of addiction, overwhelming trauma runs through each plaintiff’s testimony. Several describe physical and sexual abuse suffered as a child. One patient was born with fetal alcohol syndrome disorder. Another attended a residential school. Another is a victim of the Sixties Scoop.
One harrowing testimony recounts a moment when one of the plaintiffs, a young woman, awoke “rolled up in a carpet and at the dump.”
“I walked through the iOAT Calgary clinic a broken person,” that young woman later testified. “I had no self-worth and self-esteem. I was dead inside, and so angry at the world.”
Like Anderson and the other plaintiffs, she also credits iOAT for giving her life back. “For the first [time] ever, I can see a future for myself. A future where I don’t use drugs. A future where I can live safely without fear of dying of an overdose, contracting a disease, or being killed by others on the street.”
Staff at the iOAT clinic helped Anderson find housing. If the government defunds the program, he thinks he’ll almost certainly return to the street.
Still, Anderson supports the premier because he says he fights for the common worker. But Kenney’s stance on iOAT leaves him stumped.
“I don't think the Kenney government understands how good of a program this is. I don't think it should be shut down. I think it should be expanded.”
Patty Wilson, a nurse practitioner involved in the lawsuit, says patients in the program face an acutely high risk of overdosing if they begin using street drugs again. Not only are IV drug users more susceptible to overdoses, but as the tolerance levels of iOAT patients have dropped during their time in the program, the street supply appears to have grown even more toxic.
“It's not hyperbole to say life or death, it actually is life or death,” Wilson says. “It has never been more dangerous for them to have to go back to this.”
In anticipation of iOAT’s end, some patients have begun to disengage and slowly reintroduce street drugs into their system, a “pragmatic” move that reduces their chances of an overdose, according to Wilson.
A variable forecast
A few days after Canada’s health minister encouraged Alberta to reconsider ending iOAT, Kenney’s government suggested it may continue providing the treatment in some form. The next day, however, Luan called the program “a mess.”
Avnish Nanda, the lawyer representing the iOAT patients, is not sure what to think. He told The Tyee that the government’s legal counsel has indicated that the lawsuit may be “moot” very shortly. If so, and the government has a change of heart, Nanda thinks shining a light on the stories of the 11 patients might have moved the needle.
“Having people with opioid use disorder talk about their experience is the most compelling and effective way to address this issue,” he says.
“You hear from folks that you can identify with, that you may know, talk about how this is life and death to them. It just flips everything on its head.”
Lethbridge had its first snowstorm of autumn two weeks ago. On Monday, it felt a bit like summer again, as the thermometer nudged a high of 22 C. By Sunday night, though, it’s expected to plummet to -14, and more snow will fall on the glowing orange tent in Galt Gardens. Tim Slaney expects to be there, supporting his clients as much as he can with food, warmth and a sympathetic ear, as the police look on and any protesters who care to brave the cold hurl insults.
“I’m just trying to remind myself that folks don’t react like this unless they think that you have a shot at achieving what you set out to do,” he says. “That’s kind of my solace right now.”
Petra Schulz finds a bit of solace in this moment, too. She sees hope in the fact that the tent still stands, the lawsuit proceeds, and voices for the kind of help she thinks could have saved her son have yet to be silenced in Alberta.
“For the longest time,” she says, “we’ve just been on the receiving end of their cuts and their actions. Now people are standing up for their rights and for what they deserve. That is really beautiful to see.” ![]()
Read more: Health, Rights + Justice
















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: