Marginalized Canadians have borne the brunt of economic and social impacts of COVID-19, and new data suggests they are shouldering the mental health burden as well.
Racialized, LGBTQ2S+ and low-income people are more likely to be experiencing worsening mental health and problems coping with the turmoil of the last few months.
And they are also least likely to have the means and support to access mental health care — especially now.
“At the best of times, it can be a struggle in maintaining your care routines, your relationships with your family and your care providers, picking up prescriptions, all of those kinds of things,” said Jonny Morris, CEO of the Canadian Mental Health Association in B.C. “Compounded with the stresses of just grappling with this very new time, arguably for many it’s quite a scary experience.”
The first results from a collaborative study by two University of British Columbia researchers, the CMHA and the U.K. Mental Health Foundation have demonstrated the unequal mental health toll. The long-term study will compare results over time and compare the impact in Canada and the U.K.
Around 38 per cent of the 3,000 adult respondents reported worsening mental health overall, but that number was 59 per cent for those already dealing with mental health challenges.
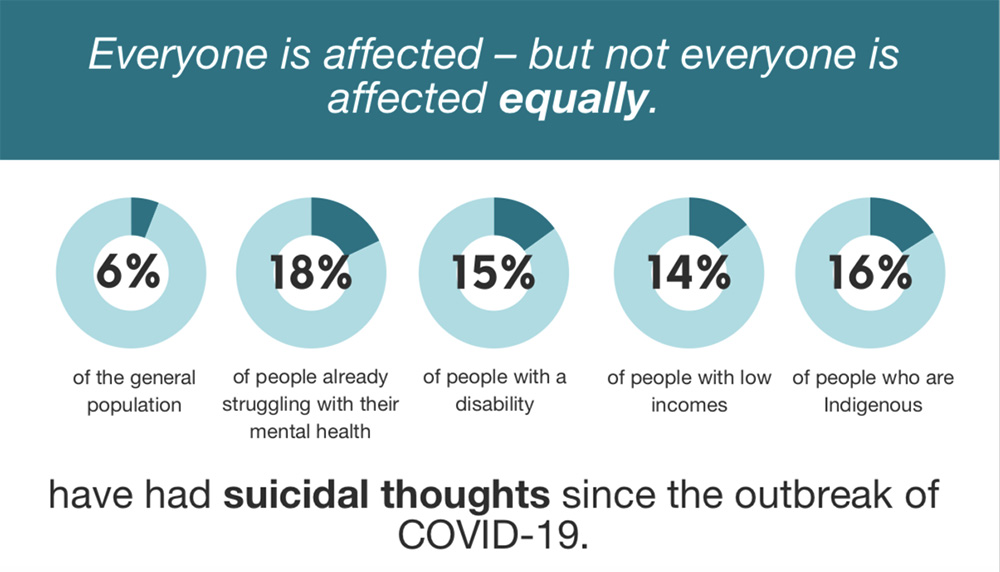
People with pre-existing mental health conditions were three times as likely to have had suicidal thoughts as the overall population since the pandemic began. People with disabilities, low incomes or Indigenous people were more than twice as likely to have had thoughts.
Only 16 per cent of people with pre-existing mental health conditions reported accessing in-person or online mental health care.
Low-income and LGBTQ+ respondents and those with disabilities were also more likely to report worsening mental health at rates between 43 and 47 per cent.
These groups were about twice as likely to report having trouble coping, compared with the 14-per-cent rate in the general population.
Indigenous and racialized respondents also reported more trouble coping at 26 and 22 per cent. And 18 per cent of people of colour reported heightened concerns about physical or emotional abuse in the home compared to seven per cent of the general population.
“We already know that there’s an impact and a wide impact... but what we were failing to do was look at the differential impacts,” said Emily Jenkins, an assistant professor of nursing at the University of British Columbia and a co-lead researcher on the study.
“And especially when these vulnerabilities overlap or intersect, we can assume that there's going to be even greater vulnerability.”
Jenkins and Morris stressed that the current public reckoning with systemic racism in law enforcement, workplaces and the health-care system is linked to the mental health impacts of the pandemic on Black, Indigenous and racialized people.
“It’s long been known that discrimination, racism, the trauma that is often associated with those experiences have profound impacts upon mental health and well-being,” said Morris.
And with new attention to systemic racism in the health-care system and the sometimes deadly role of police in wellness checks on racialized people, Norris and Jenkins said it is essential for the health-care system to change and reflect the diverse communities it serves.
Morris said colonialism and racism determine health outcomes.
“Being Indigenous is not the risk factor, the effects of colonization is the risk factor, and being Black or a person of colour or mixed race isn't the risk factor... but systemic racism and injustice are, because it leads to the experience where access to care is challenged,” said Morris.
“There's the double whammy of both stigma in grappling with a mental health or substance use problem and how one is treated by virtue of the colour of your skin or the language you speak.”
Jenkins hopes the data helps support policies that focus on the social determinants of mental health that cause marginalized populations to bear more of this burden — like income, housing, race and other factors.
“What the pandemic has really brought awareness to is that experiences with mental health challenges are not just an individual issue,” said Jenkins.
“We’ve historically drawn on the biomedical model to understand mental health, and that fails to account for the profound impact of the social determinants of health, or the everyday conditions in which we live, and how those shaped our experiences with mental health and mental health inequities.”
Morris and Jenkins are looking to make the case for mental health recovery that includes the social and economic supports essential to strong mental health and resilience.
“You can have all of the mental health treatment in the world that’s culturally responsive,” said Morris. “But if you are living precariously, or if you are experiencing violence, or if you are feeling isolated and socially disconnected, all of the mental health treatment in the world is still not going to necessarily tackle those other broader issues.”
The survey results show the need for “bold and decisive action” from government, they agree.
“Treatment alone isn’t going to fix someone’s housing insecurity or that someone lost their job,” said Jenkins. “We need to be thinking just beyond the health system and really developing a comprehensive mental health strategy, from promotion, through prevention, through treatment... to a holistic approach not centred in treatment of disorder.”
Need help? Here are some numbers to call
1800SUICIDE: 1-800-784-2433 if you are considering suicide or are concerned about someone who may be.
310Mental Health Support: 310-6789 for emotional support, information and resources specific to mental health.
Here’s also a map of crisis lines and resources by region.
![]()
Read more: Health, Coronavirus
















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: