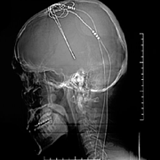
Eights months ago, surgeons drilled two holes into the skull of a wide-awake Vancouver man and inserted spaghetti-sized electrical wires down through the two sides of his frontal lobes. They left behind a remote control brain pacemaker, which regularly shocks his brain with three volts of electricity, 24 hours a day, seven days a week, powered by a battery pack that sits on his neck. The device is meant to treat his severe depression. It's part of a controversial clinical trial of a procedure called deep brain stimulation (DBS) that's jointly run by UBC and VGH, and being partly funded by B.C. health care.
As part of the trial, which is co-sponsored by a Texas-based medical device manufacturer, researchers will also implant five other British Columbia patients through a multi-centre trial also happening in Toronto and Montreal. DBS is also being tested at centres all over the globe, as a treatment for obsessive-compulsive disorder, anxiety, eating disorders, addictions and even violent behaviour. But emerging data on this new technology is raising questions about the effectiveness of the procedure, the link between health care and profits, and the ethics of quick-fix psychological treatments.
With the World Health Organization warning that depression is increasingly common and is already, globally, the leading cause of disability, proponents of DBS and other neuromodulation technologies like vagus nerve stimulation are excited about the various potential promises of these so-called high-tech neuromodulation devices. Depression is now the leading cause of worker disability in Canada. And in doctors' offices, it's the fastest-growing diagnosis, causing prescriptions for anti-depressants to double between 1999 and 2004.
Final depression frontier?
Proponents of deep brain stimulation for depression say it could be a novel way to curb the illness in 20 per cent of individuals who don't respond to front-line treatments like drugs and psychotherapies. Deep brain stimulation is meant to interrupt specific pathways between the frontal lobes and the deeper emotional parts of the brain, essentially "rewiring" the brain. It's the same physiological rationale used to describe lobotomies and their modern counterparts, known as psychiatric neurosurgeries, which are said to be making a comeback at select centres round the globe, including a UBC program started in 2000. DBS is being held up as a good alternative to psychiatric neurosurgeries, because it doesn't involve permanently destroying pieces of the brain, and because the device can be turned off.
The immediate effects of DBS are often dramatic from the moment the patient is test-stimulated while on the operating table. "Suddenly my patient started laughing and talking about eating croissants and going to aerobics class," says McGill psychiatrist Dr. Guy Debonnel about the test-stimulation of his first DBS patient through the multi-centre DBS for depression trial. Debonnel notes that even a slight change in electrical placement "can change a patient's feelings in seconds from laughing to feeling bad," and they would even say they felt like crying. Debonnel says his students "were a bit scared that the technology had the power to change emotions so dramatically."
Sad blood?
The area of the brain in question is called Cg25. The role it plays in depression started in neurologist Dr. Helen Mayberg's University of Toronto lab. She hooked healthy and depressed individuals up to brain scans measuring cerebral blood flow activity, and while they read "sad" material, activity in the Cg25 area increased. Healthy peoples' brains were able to snap out of the depressed feelings quickly, but Mayberg found that depressed people "were swamped by this emotional state and found it impossible to motivate other brain areas. With depressed people there's a tug-of-war between emotion and thinking," says Mayberg.
Mayberg acknowledges that neuroscience has yet to find a clear anatomic abnormality in depressed individuals, and that brain scans can't read significant increases or decreases in blood flow, but she was able to get permission to start a proof of principle research trial with DBS. "Good news, it gave us very promising results." She said 66 per cent of the patients had significant improvement. All of them were "very disabled" before the surgery and hadn't responded to medications, electroconvulsive therapy and psychotherapy for at least five years.
"Fifteen per cent of these individuals will commit suicide without treatment," says Mayberg, "but after DBS, many are back at work."
Post-operative psychological tests of the Toronto patients showed no negative cognitive and behavioral effects, though various studies elsewhere have linked the types of blood flow changes seen in DBS patients to mania, dementia, lack of response to aversive scenes and serious psychiatric personality disorders like depersonalization and psychosis. Long-term follow-up will be necessary to see whether physiological damage to the brain and the central nervous system occurs as well. The Toronto group has yet to publish data on post-operative neuropsychological tests, but their initial paper contends that none of the patients had cognitive impairments or adverse behaviour changes.
Light bulbs
In Toronto, after researchers published the results of their first study, over 300 people with chronic depression wanted to sign up for DBS. A few patients spoke to the media after their operations, and credited the benefits of the procedure. One Toronto patient described it as if a light bulb had been turned on. She said that upon returning home from the hospital, she threw on a hat to cover the surgical staples, and went straight out into the garden to clip the hedges. Others said they were finally able to get out of bed and start living their lives, returning to work and school.
Reports from other centres doing DBS for obsessive-compulsive disorder showed similar success rates. Though they reported two downsides: the battery packs had to be surgically replaced within five to twelve months due to the high voltage rate. And the treatment failed altogether for two of the patients, who went on to receive irreversible psychiatric neurosurgeries.
There have been other questions raised by the results of the surgeries. One European patient treated for social anxiety was so enthralled by her improved mood that she asked her psychiatrist to turn up her voltage for a weekend social event, hinting at the potential off-label use of this type of technology to tweak performance in high-functioning individuals like athletes and brain workers, or even inhibit violent behaviour in criminals.
'Unperfected'
The UBC team acknowledges the various ethical issues and says strict guidelines and protocols are in place. "We're flying into pretty complicated territory here. The process is unperfected," says Dr. Andrew Howard, a UBC psychiatrist who is responsible for meeting with the DBS trial patients weekly to fine-tune their electrical implants with the remote-control computer devices stored at his office. "This could be a new dawn for psychiatric neurosurgery, but considering the horrible history, we can't repeat those mistakes."
"We don't know how the technology works, whether it's stimulating or inhibiting the brain," says Dr. Chris Honey, the VGH neurosurgeon doing the local surgeries. "We're in the honeymoon stage right now, but that might end," he adds, particularly since the mechanisms of deep brain stimulation, and the workings of the Cg25 target are little-known, though clinical studies have linked it to moral decision-making, and tissue damage in the area has been associated with disinhibition, which is associated with frontal lobe brain damage causing negative behaviours and poor impulse control.
Bio-ethicists and psychologists are also concerned about the procedure, due to the corporate moneymaking potential. The neuromodulation market is already said by one firm to be worth about $3 billion US and is forecasted to reach about $8 billion by 2010.
Dangerous cures
Recent studies on DBS show that this technology also comes with many adverse side effects. In Canada, DBS has been used to treat Parkinson's disease since 1997. And clinical studies from these treatments have chronicled various dangers, including stroke and death from the surgery along with post-op cognitive deficits, suicidal tendencies and negative personality changes ranging from mania to depersonalization to criminal activity.
"Brain surgery for mental disorders should have gone out with stone age trepanation (boring holes in the head)," says Dr. Alan Baumeister, chair of Biological Psychology at Louisiana State University.
Dr. Baumeister has done extensive research on the checkered history of neurostimulation, then known as Electrical Brain Stimulation (EBS). Baumeister is concerned about the recent chatter amongst psychiatrists, neurologists and neurosurgeons that psychiatric neurosurgeries are ready for a comeback as a last-resort treatment for mental disorders. He says the same thing happened when the frontal lobotomy was introduced in the 1930s, before the treatment was restricted in the 1970s (after over 50,000 lobotomies were performed in the U.S. alone). "So, to say the least," adds Baumeister, "I am dubious about DBS."
Dr. David Roy, founder of Montreal-based Centre for Bioethics agrees. "Horrific, ethically unacceptable experiments happened in the past around psychiatric neurosurgeries and brain stimulation, supported by major medical journals and governments." He says once again, there's a high enthusiasm for DBS as a treatment for mental disorders without evidence of significant benefits, and warns that the enthusiasm could "lead us into a new wave of abuse."
Talk, drug or cut?
Francoise Baylis, a Dalhousie-based neuroethicist has another concern: the funding of the UBC study. The surgery itself is being covered by government health care funds. She says that typically, the health care system doesn't pay for clinical trial research, and that drugs, devices and procedures need to be thoroughly clinically tested before taxpayer dollars are spent funding them. "We need a healthy dose of skepticism about these neurotechnologies and approval policies. Everyone is vulnerable: the institutions looking for access to grant money, and the patients."
Dr. Mayberg, who now works at Emory University in Atlanta, acknowledges that, "In the U.S. we have a lot of hurdles [with DBS trials] that you don't have in Canada. We couldn't do here what we did in Toronto, since, in the U.S., the expectation around research trials is that the manufacturer will pay for everything."
Dr. Wolfgang Linden has a different set of concerns about the implications of using surgery rather than cognitive approaches like talk therapy. "Many depressed individuals grew up in dysfunctional families or have had really negative experiences in their lives," says Dr. Linden, a UBC psychology and president of the BC Psychology Association. He says treatments like these take a black and white approach to treating mental illness and ignore core psychological issues. He adds that the government under-funds psychology, and that only about five per cent of the B.C. population has access to psychotherapies, mostly through private insurance. "If you work for McDonald's, forget about it."
Prescribing sanity
Linden points out that many clinical studies have shown that people who receive cognitive behaviour therapy are more likely to curb depression long-term than people who take medication, but they're "under-treated with these time-tested treatments" and end up at their GP's office looking for help which too often comes in the form of a drug prescription.
Dr. Lam stresses that "the patients undergoing DBS have already failed cognitive therapy and other psychological treatments in addition to biological treatments," and he contends that, "It is never a simple question of either/or." He cites the analogy of "heroic and invasive" treatments for people with severe cardiovascular diseases, "even though we know that funding exercise programs and dietary programs can prevent many of those diseases."
The UBC team initially told The Tyee that their first patient had yet to "respond" to the DBS treatment. His condition is currently unknown, as UBC is not releasing information to the media and will not report whether any other patients have since received the implant. Dr. Howard has said that whether the first patient responds or not, they plan to proceed with DBS for another five patients.
"Only in dramatic cases do we hear about things going wrong in clinical trials," says Michael McDonald, founding director and chair of UBC's W. Maurice Young Centre for Applied Ethics. "We shouldn't impede research but we should make sure to protect citizens. I can tell you exactly how many animals were researched and exactly what happened to them, but we have no national database for human medical trials. That sure says something about our culture."
Related Tyee stories:
















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: