Thomas Hartle speaks with a pronounced cheeriness that’s initially hard to reconcile with his words. “I'm honestly trying to do my very best to die with cancer,” he says. “Not from cancer.”
That hasn’t been easy since Hartle was first diagnosed in 2016. Surgeries and chemotherapy did keep his stage four colon cancer at bay, but the tumours returned last summer. It’s now inoperable. The spikes of abdominal pain led to a new problem — “High anxiety levels in terms of panic attacks on a daily basis.”
Hartle is just 52, and unwilling to let fear claim the time he has left with his wife and two children. Being a self-described “professional nerd” and an IT professional, Hartle says he’s drawn to research. He found a Johns Hopkins study that reported 80 per cent of cancer patients involved achieved significant clinical decreases in depression and anxiety using psilocybin, the psychoactive compound in magic mushrooms.
Although psilocybin has been illegal in the U.S. since 1968 and banned in Canada since 1974, Hartle discovered that Therapsil, a non-profit based in Victoria, B.C., was working to make the illegal psychedelic available to palliative care patients using Section 56 of Canada’s Controlled Drugs and Substances Act. It allows the federal health minister to grant exemptions from drug laws if “necessary for a medical or scientific purpose or is otherwise in the public interest.”
That’s how Insite, North America’s first supervised drug injection site, opened in Vancouver in 2003. In 2017 Health Canada began granting Section 56 exemptions to the Santo Daime church to import and use ayahuasca as a sacrament. Ayahuasca is a herbal tea with naturally occurring — and illegal — dimethyltryptamine, or DMT, similar to psilocybin.
So Hartle joined a queue of applicants, shepherded by Therapsil, asking the government for permission to use psilocybin for palliative care patients.
Last August, after months of lobbying, federal Health Minister Patty Hajdu granted exemptions for Hartle and three others on compassionate grounds.
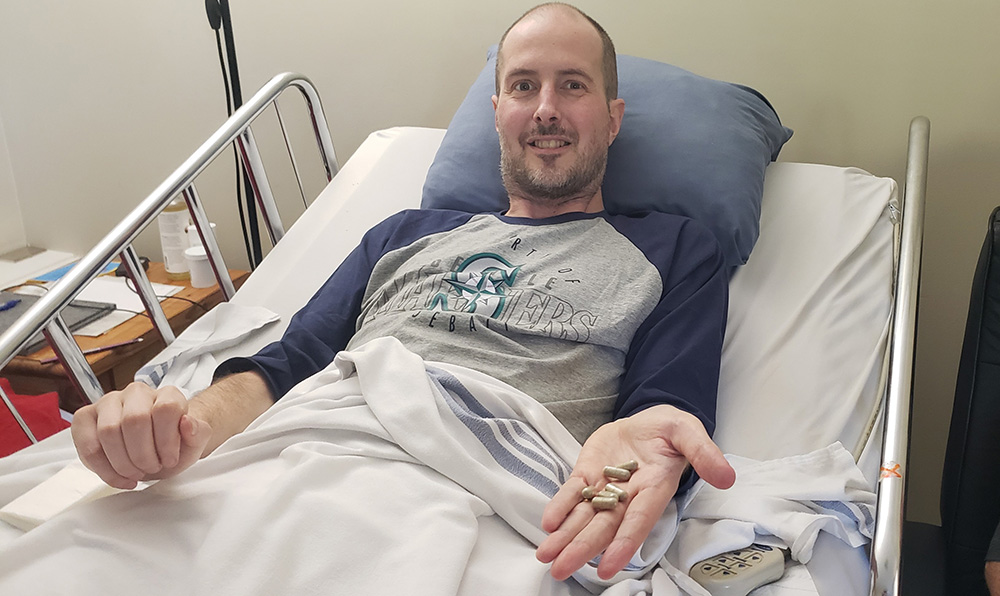
A week later Hartle lay in a bed in a spare room at his home in Saskatoon. He donned a sleeping mask and headphones. He took seven grams of dried powdered magic mushrooms. Asking him to describe the next six or seven hours, is a bit like asking someone to describe a colour that doesn’t exist.
“So the music that I was listening to created very immersive three-dimensional spaces,” he recounts. "I was not in those spaces I was experiencing though. I was those spaces.”
Three months later, Hartle is still profoundly changed.
“All the busy, useless sort of thoughts that you get with anxiety have become very quiet for me,” Hartle says. “It’s so much easier for me to remain in the present moment and that's greatly improved the quality of my life. So now if I get a pain or something like that, it's discomfort and I don't enjoy it. But I don't immediately go to you know, ‘Am I gonna die this afternoon?’”
Hartle can describe his psilocybin experience at some length and detail. And even though I have had several sessions of psychedelic psychotherapy myself, the best I can do is listen and nod. It takes a therapist with experience in the power of psychedelics to help the patient plan their intentions for the trip, and to draw meaning from the result. Hartle’s Section 56 exemption was undoubtedly successful in part because he had a trained psychotherapist supporting him.
Therapsil’s founder, clinical psychologist Bruce Tobin, flew to be at Hartle’s Saskatoon bedside for that first dose.
“We’re very much a believer in the idea that when a traveller wants to go through an unknown mountain range, they would choose a guide who's been there before who can help them,” Tobin says.
Tobin, based in Victoria, has been practising for four decades. He grew up in the hippie age and had his own experiences with psychedelics before they became illegal.
“I had the good fortune of knowing one or two people who had received professional treatment with a psychedelic in a hospital near Vancouver,” Tobin says, adding that while traditional drugs like antidepressants have their place, they don’t always work.
“There are a number of major mental health issues including anxiety, depression, PTSD and addiction.” Tobin says. “There's a whole range of patients for which we have no really effective treatments.”
There’s a reason for that, according to Dr. Sean O’Sullivan, an Ontario physician and Therapsil’s medical director.
“I'm also old enough to have practised medicine when psychedelics were legal entities,” O’Sullivan says. He says he witnessed their value for patients with depression and alcoholism firsthand in medical school in Dublin.
“Most of the drugs that are used in psychotherapy are symptomatic treatments,” O’Sullivan says. “In other words, they are suppressive medications. They suppress symptoms and they suppress neural pathways that give rise to these.”
Psychedelics like psilocybin are the exact opposite.
“Psychedelics open the doorways of the unconscious and allow previously repressed material to emerge into consciousness. The psychedelic session is a raging river sometimes and you don't want to try and stop the river or get in the way of the flow. You want to let it go through.”

O’Sullivan says therapists untrained or unfamiliar with the emotional river which psychedelics can produce are liable to be unhelpful.
“So, when people cry or weep or express rage or joy or bliss in a psychedelic session,” O’Sullivan says, “the volume is really turned up. So, if someone looks like they're really, really, really, really suffering, a compassionate therapist might want to intervene and offer comfort and support and say, ‘there, there. It's going to be all right.’”
O’Sullivan says what’s required however, is to help the patient to go deeper into the river, not scramble for the bank.
“So keeping your hands off patients and encouraging them, helping them through difficult passages and then letting them go back inside… that is the job of a psychedelic therapist.”
And it’s a difficult job, requiring upwards of 30 hours for just one session, because of the advance preparation, the time the patient spends in the experience and the extensive reintegration that occurs afterward.
Right now, there are only three doctors and therapists working with Therapsil who are comfortable doing psilocybin sessions. That was barely workable in August when just four patients were given the legal right to use magic mushrooms as part of their treatment. But the number of exemptions grew to 12 by mid-November. There are 50 more applications in the hopper. Another 50 could arrive next month.
Therapsil plans to begin training therapists next year but it wants each of them to undergo their own psychedelic experience, so they know firsthand what their patients go through. To that end it has asked Health Canada to grant 19 otherwise healthy doctors the same exemption as the dying patients.
It’s a move that is controversial, and could help explain why Health Canada still hasn’t made a decision on the applications more than five months after receiving them. The pandemic response may also have sidelined them. Health Canada hasn’t publicly explained.
In response to a number questions about the process and the time it’s taking to decide, Health Canada responded to The Tyee with a general statement that the department is “taking into account all relevant considerations, including evidence of potential benefits and risks or harms to the health and safety of Canadians,” and that “assessments are done as quickly as possible.”
One question likely being asked inside the department is why psychedelic therapists are any different than psychiatrists, who prescribe powerful antidepressants without having taken them.
O’Sullivan says a more apt comparison is to consider traditional psychotherapy. You wouldn’t seek treatment from someone who’d never experienced it as part of their training.
“If you as a therapist have not had any exposure to those realms of the human unconscious,” O’Sullivan says, “then you are apt to do what most people would do in these circumstances. You would either trivialize them or you will pathologize them, rather than looking at them as rich sources of information about the person's unconscious.”
Christian, a 43-year-old cancer patient on Vancouver Island who didn’t want his last name used, puts it more simply.
“It's like any profession. If you take your car to a mechanic, you want them to have driven before.”
Two years ago, Christian’s workaholic life as a consultant helping startups with accounting and procurement in China hit a wall. His mother had died of breast cancer, he and his wife had been evicted from their apartment, and he was diagnosed with stage four rectum and liver cancer. Palliative care counselling offered through BC Cancer helped some. But by last August, pain had confined the six-foot-four formerly active go-getter to his bed for more than 20 hours a day.
“Just to get out of bed now to go to the commode two feet away is like a half-hour endeavour,” he says.
And cancer had allowed his fears to gain a foothold.
“I'm afraid of dying too quick. Not being able to provide for my wife,” he says. “It's difficult for me to think of what if I go in one month... what happens to her then?"
Christian says he is a believer in alternative therapies. After reading about the Section 56 exemptions last August, and with the encouragement of a counsellor, he emailed Therapsil.
Two months later he received his own legal permission to use psilocybin. He thinks he was lucky because Therapsil’s founder and main therapist Tobin lives just five minutes away.
“Realistically they can only help people in Kelowna, Toronto or here in Victoria,” Christian says, referring to where Therapsil’s trained therapists are currently based. “If I was in Nanaimo or Campbell River I might probably have died before any of this ever happened.”
Therapsil’s CEO Spencer Hawkswell says they’ve already had to deal with that situation.
“Over Labour Day, we had a woman who was dying reach out to us, and she had probably less than a week to live,” Hawkswell says. Even though Therapsil says Health Canada is now approving exemptions for patients in about 10 business days, it’s not fast enough. The woman died.
And Hawkswell suggests that without more properly trained therapists, that may be a common outcome.
“You know the rate at which we will be able to treat patients is probably one a week.”
Therapsil says it already has a fairly conservative treatment criteria that rejects people with pre-existing mental health conditions involving schizophrenia or psychosis. People on several antidepressants can also be disqualified if they can’t be weened off them because those drugs severely blunt any psychedelic effect. Even with those restrictions Therapsil estimates about 2,800 new terminal cancer patients a year could qualify for the treatment.
Yet rather than pause the process or become more restrictive, Therapsil opened up its criteria, at least temporarily, by helping to secure the first exemption for a patient who is not terminally ill.

In early November Mona Streleaff of Victora underwent a session to help her deal with debilitating depression and PTSD that has its roots in her childhood growing up in Finland. “My mother was bipolar. My father was an alcoholic and he used drugs. So, there was a lot of anguish in my household. I don't need to go into detail, but there was a lot of anguish.”
In 2002 Streleaff had bilateral breast cancer, which eventually went into remission, but it left her traumatized.
“I was 48-years-old at the time”, she says. “I had six grandchildren and it was very tough to be facing death.”
A couple of years ago her daughter died in a car crash.
“The depression… got very, very terrible after I lost my child,” she says. “I started drinking like there was no tomorrow. I think I was actually trying to commit suicide.”
Streleaff says years of pills, talk therapy and treatment centres didn’t help.
It just so happened that Therapsil’s founder is also her therapist. Tobin conducted Streleaff’s psychedelic therapy in her home.
“It's not something like what the kids would think about you know, ‘let's have some psychedelics and go and get high and have some fun,’” Streleaff says.
“This is therapy. It's difficult. It’s hard work. There’s a lot of emotion that is extremely hard to face. There's sorrow. There's grief. There is anger. But there is also empathy, compassion and forgiveness.”
A week after her four-hour trip fuelled by psilocybin tea, Streleaff says she’s anxiety-free.
“I've been calm. I'm more alive than I've been for a while.”
Not everyone is guaranteed the same breakthrough. A few days after Christian’s session he thinks it wasn’t as profound as he’d hoped.
“I was like in and out of different realms,” he recalls, “I would open my eyes and then see people around and ask for my wife and ask where she was or I would look at her and not necessarily see her there.”
But Christian suggests his obsessive-compulsive personality may have fought against the raging river O’Sullivan talks about, rather than letting it carry him.
Even so, Christian says he’s noticed changes. Cancer has kept him bedbound most of the day and to cope with anxiety he would be on his smart phone incessantly. “This morning for example,” he says, “the home care worker who comes and cleans me every day mentioned it was the first time she'd seen me reach for my phone in over an hour.”
Christian says the persistent anxiety he felt prior to the experience has abated. It’s an experience he might try again, as his government exemption, delivered via email, is good for one year.
Advocates of psychedelic therapy argue the exemption process is not a solution. While it does free the holder from fear of arrest or prosecution for possessing and using psilocybin, Health Canada’s wording is quite clear that it doesn’t apply to selling and procuring.
Canada’s compassionate nod to the dying is less progressive when held beside legislation in several U.S. states to decriminalize magic mushrooms. In Oregon, voters overwhelmingly backed a ballot initiative this month to create a state-licensed psilocybin therapy program.
Tobin says Health Canada’s approach so far has been to ask applicants where they intend to get their mushrooms.
“One applicant said, ‘I'm growing my own right now.’ He got his approval. Another patient said, ‘I plan to get them from a trusted friend and that's all I'd like to say about it.’ She got her exemption."
“People who take mushrooms on a Friday evening with six beers… they don't give a tinker's toss about the law,” O’Sullivan says. “They're not concerned about it, but they are not the people who are coming to us.”
O’Sullivan says the people looking to Therapsil just want help.
“We've got a 45-year-old woman with cancer that’s spread to her bones. A 53-year-old woman with cancer in her bones and her brain. We have young people with soft tissue malignancies. They're not interested in breaking the law and I really think that our government recognizes this.”
Right now, it isn’t the law that’s holding back psilocybin psychotherapy. It’s money.
There aren’t enough therapists. Training will take funding. Therapsil plans to launch a GoFundMe campaign to raise $500,000 to underwrite its plans. CEO Spencer Hawkswell says an anonymous donor has offered to match up to $250,000.
If successful, he says they’ll expand their intake of patients to include more non-palliative cases like Mona Streleaff. Tobin says that won’t change the non-profit he founded as a humanitarian patient advocacy organization.
“We will never offer stock. We will never have investors. We have a small paid staff that earns a reasonable living wage but beyond that Therapsil will never see profits and I myself as founder am committed to never receiving a penny from any of this.”
Compared to the hundreds of millions of dollars raised for cancer research in Canada each year, Therapsil’s financial goal seems microscopic.
But unlike cancer agencies, Therapsil can’t hold out the idea of finding a cure. At least not in the traditional sense. There is no potential that psilocybin psychotherapy will trigger miraculous remission by repairing the psyche. O’Sullivan say it just doesn’t work that way.
“I had a child who died of cancer when she was seven years of age,” he reveals. “She was a bright little angel of light to the world. She had no psychological issues that made her get cancer. So no… it's not an attempt to prevent death. It's an attempt to help people die well.” ![]()
Read more: Health, Federal Politics















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: