New Pandemics, Old Politics: Two Hundred Years of War on Disease and its Alternatives
By Alex de Waal
Polity Books (2021)
“Anagnorisis” is Greek for “learning upward” — the sudden shock when we finally see and understand what’s really going on. I had such shocks on almost every page of this very important new book. This is a long review because the book raises very many issues rarely mentioned in medical or political history. It calls into question not only our global health system, but the economic and political systems that pretend to support it.
Alex de Waal is the executive director of the World Peace Foundation at the Fletcher School of Law and Diplomacy and professorial fellow at the London School of Economics. He is an expert on the politics of Sudan and the Horn of Africa, and the author of seven previous books on Africa, AIDS and famine. He is also writing sharp analysis of the war in Tigray that attracts a lot of critics on Twitter.
I may believe his critics when they document their charges as well as de Waal documents his case in this book. And that case is that the world system we have built over two centuries of imperial conquest and rule is itself the generator of pandemics; the pandemics emerge from our politics and economics, and we respond to them politically — not medically. This essay draws on de Waal’s book to trace various ways societies over the ages have misunderstood and poorly responded to plagues in their midst. I’ve selected five myths that persist today.
1. PLAGUES ARE JUST BAD LUCK
A key insight, de Waal argues, is the language of pandemic response. War has got us where we are today, and war remains the metaphor for dealing with non-military threats to social stability. Citizens have been exhorted to make wars on drugs, poverty and climate change. And today’s leaders, with few exceptions, have declared war on COVID-19, on describing the response as a “fight,” and the health-care workers as the “frontline” or even “warriors.”
Such military imagery would have made no sense in the wars of the 18th and early 19th centuries, when disease was endured but not fought. Sickness always killed more soldiers than combat, but the generals took that toll as a cost of doing business. George Washington was ahead of his time in requiring his soldiers to be vaccinated against smallpox. Most European powers considered disease outbreaks as just bad luck, about which little could be done.
The modern pandemic age began with cholera in the early 1800s. It was a known but tolerable disease on the coast of the Bay of Bengal, but development by the East India Company spread it across much of India. Ever-increasing trade and travel between India and Europe carried cholera west and north, into the heart of the industrial revolution. Clean water and sanitation had not been seen in those regions since the fall of the Roman Empire, and cholera tore through working-class slums.
Yet governments still saw this as more bad luck, not bad policy. They saw no reason to deal with cholera beyond reducing a hindrance to business. When cholera threatened to spread westward into Prussia, troops were sent east to establish a cordon sanitaire blocking migrants. Both the commanding officer, August von Gneisenau, and his chief of staff Carl von Clausewitz (the great military theorist) died of cholera.
Strikingly, de Waal notes that neither Carl von Clausewitz nor Karl Marx took any note of disease as a factor in war or politics; disease was just there, like the weather. Communism and capitalism alike were blind to one of capitalism’s greatest flaws: Running as intended, it created social and hygienic conditions that killed people. It had to. It couldn’t make a profit otherwise.
The British Empire finally took some crude public-health measures to keep cholera out of Europe: quarantine stations at the Suez Canal, for example. But the prosperity of the Raj depended on the poverty of India, and the British weren’t about to spend money to provide the natives with clean water and sewage.
“Between 1817 and 1865,” de Waal writes, “cholera killed about 15 million Indians. Between 1865 and 1947, it killed 23 million.... For 30 years after the last cholera deaths in Britain, perfidious Albion maintained an entirely different set of doctrines for cholera control — as well as respect for basic humanity — east of Suez.”
The last cholera outbreak in Europe arrived on a train from Moscow in August 1892, whose passengers were Jewish artisans expelled by the tsar. That political act provoked completely political responses. The First Reich, established after the Franco-Prussian War, had not yet established uniform control over the old German patchwork of independent states. Hamburg, like a pro-Trump state government, denied the cholera threat, suppressed the news, and let 10,000 residents die: “They believed in small government, balancing the books and individual responsibility for health and well-being.” And they didn’t want to declare an outbreak because it would shut down shipping in and out of Hamburg. Then as now, the economy took priority over people’s health.
Moreover, the germ theory of disease was as contentious as COVID-19 vaccines are today. The Kaiser’s health expert was Dr. Robert Koch, who had identified the bacteria that causes cholera, while other German researchers still argued for “miasmas,” or tainted air. Another medical titan, Rudolf Virchow, dismissed the germ theory and blamed social conditions for disease: “Medicine is a social science, and politics is nothing else but medicine on a large scale.”
On the Kaiser’s authority, Koch took over Hamburg. He purged both the city’s health-care authorities and its water system, and ordered patient isolation. The outbreak ended in September.
But Germany and the world learned the wrong lessons: Outbreaks were the result solely of germs, not miasmas or social conditions like poverty and overcrowding; a “war” on disease was an excellent pretext for extending and enhancing the power of the state over its communities.
2. PLAGUES ARE ENEMIES OF WAR
Koch’s success, de Waal argues, set the pattern: “This was the ‘war on disease’ narrative, in which science and military-style public health would fight and conquer an invisible enemy.” As Clausewitz might have put, if he’d lived, “public health is an act of force to compel our enemy to do our will.” Thereafter, the enemy was not only the disease, but the community it afflicted.
It was a storyline we still follow: “Its first element was the plan of campaign — an assemblage of instruments for social control, which we could distil into a slogan: lookout, cleanup, and lockdown.… The next operation in the war story was conquest and dominion.… The final element was the technology for victory, when microbiologists began crafting ‘magic bullets’ that could hit those invisible enemies.”

The war story also worked for the conquest of yellow fever after the U.S. victory in the Spanish-American War in 1898. That opened the way for the Panama Canal, where a French attempt had been beaten by mosquitoes. Medical science, backed by government, enhanced American imperial power under the proudly racist president Teddy Roosevelt. He wanted to project American power in regions where only the resident non-whites had some immunity to local diseases.
As the leader of the yellow-fever campaign, Dr. William Gorgas told a graduating class of medical students at Johns Hopkins University, “Our sanitary work at Panama will be remembered as the event which demonstrated to the white man that he could live in perfectly good health in the tropics; that from this period will be dated the great white civilization in these regions.”
But the war story failed altogether in the 1918-19 influenza pandemic. With a war already under way, flu became a distraction. Neither side wanted to talk about it, and president Woodrow Wilson (who never once mentioned influenza) kept pulling young recruits into crowded training camps and then shipping them on crowded trains to crowded ships bound for France. They died en route in thousands.
Perhaps as many as 60 to 100 million people died around the world, including many here in B.C. The vast majority were non-whites in Asia, Africa, Latin America and North America’s Indigenous reserves and residential schools. The imperial states barely noticed. COVID-19 in a similar time period has killed about four million — surely an undercount, but still a small fraction of pandemic influenza’s toll.
Wilson himself evidently came down with flu at the Paris Peace Conference in 1919, and suffered neurological consequences: he lost the will to impose his Fourteen Points peace plan on his vengeful European allies. The Treaty of Versailles put Germany into a dead end that Adolf Hitler used as a pretext for a still greater war.
Influenza didn’t fit the war story that Robert Koch had scripted. After killing tens of millions, it vanished as mysteriously as it had arrived, and a profound silence fell over the worst pandemic in history. My grandparents, with my father and mother in their cradles, must have been terrified. But like many war-traumatized soldiers and civilians, they never talked about it.
Despite influenza’s victory, western governments and generals learned a lesson — about how to kill human enemies more effectively. This arose from their realization that influenza had evolved into a killer in the crowded, filthy world of the trenches, aided by other diseases like lice-borne typhus. Beat disease, they saw, and you can make war everywhere.
“Suppression of typhus,” de Waal says, “probably did more to make 20th-century warfare possible than any other single innovation. The epidemiological limit on war-waging had been lifted, allowing far larger armies to be deployed in the field in conditions that would have been disease traps just a few years earlier.”
3. PLAGUES DON’T PLAY FAVOURITES
Africans were faster learners. For people at the bottom of the imperial societies, trust in imperial medicine was non-existent. De Waal describes how Black South Africans responded to the influenza pandemic. They had seen devastating outbreaks of European smallpox, and Italian-introduced rinderpest had destroyed their cattle. Influenza was just another imperial import, moving along imperial railways and into work camps. Those who stayed in remote villages were least likely to fall ill, and few returned from white-run hospitals. Good public health, to Africans, was a matter of staying the hell away from imperial health systems.
We date the HIV/AIDS pandemic to 1981 when gay American men began to die of it. But de Waal says it first jumped from a chimpanzee to a human in Cameroon in 1920 or even earlier. From there it slowly migrated through French Africa and into the Belgian Congo, noticed only as a tropical disease affecting African railway workers in the 1930s. It would not be recognized until it began affecting white people in North America 50 years later.
Even so, de Waal says HIV/AIDS might have fizzled out early. But he thinks the French colonial health-care system probably hastened its spread through a series of top-down immunization campaigns for various diseases, in which needles were rarely if ever properly sterilized.
Throughout the 20th century, many of Africa’s imperial rulers deployed workers where needed, as cheaply as possible. This meant taking men from their families and dumping them in labour camps, with their sexual needs serviced by a roving corps of prostitutes. Once HIV/AIDS was established, imperial labour policy let it spread easily through the camps, and eventually back to the workers’ own families. Regions that had such camps endured AIDS; those that did not, largely escaped it.
When Belgium abandoned what’s now the Democratic Republic of Congo in 1960, it left a vast region with no civil service. Thousands of French-speaking Haitian government officials were seconded to Kinshasa to train the Congolese; just one of them seems to have gone home in 1966 with HIV. Even that case would not have spread, de Waal suggests, without the help of a crooked blood-services company run by a crony of Haitian dictator François Duvalier. When we finally noticed AIDS 15 years later, Haitians joined gay people among the stigmatized.

Here is where the imperial war story meets a serious counter-narrative. No one wanted to fight a disease affecting gay people and Black foreigners, because the system was designed for straight white Americans — not for queers and people of colour.
Ronald Reagan was as silent about AIDS as Wilson had been about influenza. Imperial public health was about protecting upstanding white people, especially if doing so made white politicians look good. HIV/AIDS was instantly stigmatized as a problem of fringe groups who had brought it on themselves with their crazed sexuality and unsanitary lifestyles.
The fringe groups fought back. Gays kicked their closet doors down and learned the only language politicians understand — political force. Black communities fought back too. Just 40 years later, anxious white politicians smirk and wave in Pride parades, and anti-retroviral drugs have begun to reduce a pandemic to a merely tedious health condition.
This was not thanks to an AIDS war story, de Waal makes clear. The afflicted communities took public health into their own hands and told their own war story, in which the local regime and its doctors were the enemy.
4. PLAGUES ARE VANQUISHED IN HOSPITALS
When Ebola broke out in West Africa in 2014, the West saw a chance to redeem its war story and look good to the continent it had exploited for five hundred years. Like an imperial power attacking a local insurgent, the U.S. under Barack Obama sent in horse, foot and artillery to save the nations of Guinea, Sierra Leone and Liberia (the last two were creations of Britain and the U.S. as dumps for unwanted Black people from Nova Scotia and America).
The 101st Airborne even went in, and the Americans built lovely treatment centres that never saw a patient, because the West Africans rightly regarded such centres as health hazards.
After the last few centuries, West Africans have a keener perception of reality than most of us. They saw Ebola moving through the region, and they saw it concentrating on its few and undersupplied hospitals. West Africa lost a generation of health-care workers who died of Ebola as fast as their patients.
Africans didn’t need Twitter to get the word out: In western-style hospitals and treatment centres, you were as likely to contract Ebola as to recover from it, and you would likely die alone without your family — a horror worse than death itself.
So it’s no surprise that in the West African Ebola outbreak people stayed away from hospitals — and often fled from them once there. Others stayed away as well, including pregnant mothers and mothers with children needing routine vaccination, or routine treatment for diarrhea. Like any pandemic, Ebola inflicted mortal collateral damage on those it never touched.
And it’s no surprise that even well-meaning organizations like Médecins Sans Frontières saw their Ebola treatment centres attacked by mobs of angry young men. At the time, I thought the guys were ignorant dopes, but I was the dope. The guys had listened to their grandparents’ horror stories. They saw western medicine as no gift from benign white saviours.
Local governments using western lockdown methods soon learned they didn’t work. Liberian President Ellen Johnson Sirleaf tried to seal off West Point, a Monrovia slum. Her nervous troops then fired on the protesting residents and killed Shaki Kamara, a 16-year-old who bled to death from a shattered leg. Sirleaf apologized and ended the lockdown.
Eventually West Africa’s Ebola outbreak receded, after western agencies tried to understand local culture and deal respectfully with it. But de Waal notes that locally initiated responses, like simply sealing off a community as Canada’s Indigenous communities have done in the COVID-19 pandemic, worked at least as well as western medicine. You just had to hunker down, and forget about western magic bullets.
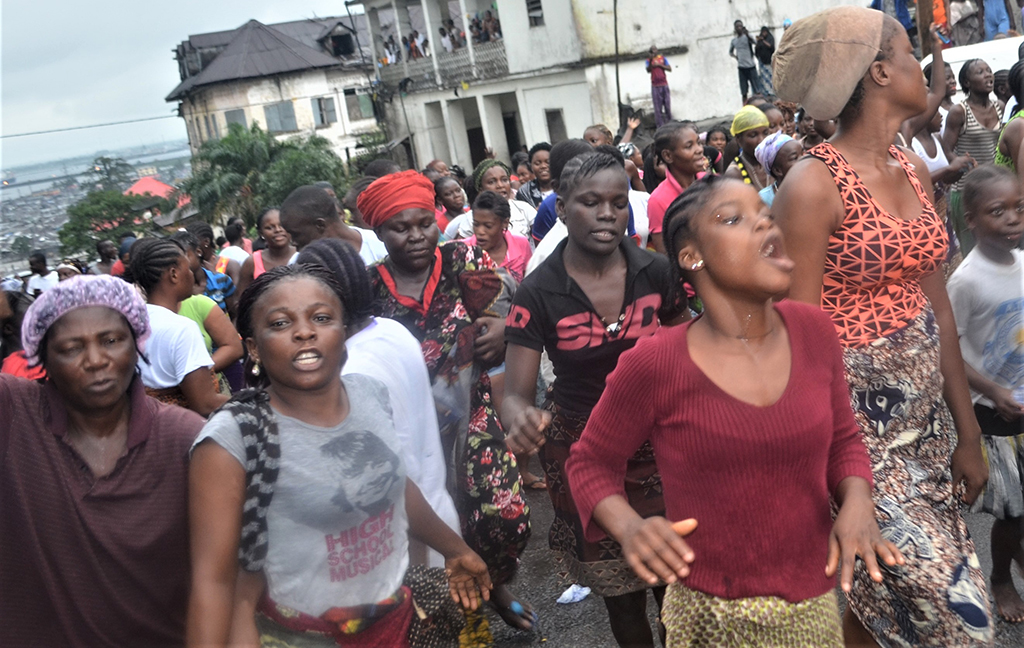
After Ebola, we began to think more about the prospects of a global pandemic while other diseases emerged: Zika virus, Middle East Respiratory Syndrome and new strains of avian flu like H7N9. Dengue, long confined to the tropics, began to turn up in Florida as a souvenir of Caribbean holidays and a portent of climate change.
Health experts realized they couldn’t ignore or deny the next pandemic; they would have to go back to the war story. Containment and “non-pharmaceutical interventions” would have to do until arrival of the magic bullets of vaccines and drugs.
The planners worked out the shape of “Pandemic X,” and while it was scary, the U.S. in particular seemed best prepared to meet and defeat it. The Americans had the most advanced health system in the world, backed by a research system that had headhunted the best and brightest from around the world.
5. PLAGUES WILL BE DEFEATED BY SCIENCE
What the planners didn’t plan for was political masters more interested in demolishing government institutions like public health.
The radical-capitalist subversion of American democracy likely began in the early 1970s. But it took decades to bring the world’s superpower to its knees under Donald Trump — a failed capitalist, but an effective radical who gained power by attacking government not just as a “problem” but as an enemy. He intended to retain power by still more attacks.
According to de Waal, Trump represented a faction of the American right wing inspired by Ayn Rand; it saw any kind of government institution as a barrier to personal freedom, wealth and social mobility. “The Trump administration,” he writes, “set out to dismantle or weaken every regulatory or scientific institution it could, and that included the pandemic preparedness apparatus built by his predecessors, both Republican and Democrat.”
And while Trump may have fallen seriously ill with COVID-19, he used even that to downplay the threat. As de Waal also observes, “The novel coronavirus isn’t the nemesis of radical capitalism — the two parasitize on one another’s disruptive politics.”
Trump drew many of his followers from the same kind of alienated underclass that attacked Ebola treatment centres in Africa: they saw government as a remote and coercive power. Doctors had sold them on the opioids that killed them, their wives and their children. Booze and tobacco were their fatal comforts. Lack of education had locked them into squalid lives and deaths of despair.
So we should not be surprised that, well into the second year of the pandemic, such followers still think it’s a hoax even when their own family members are being intubated and then dying.
Those followers may be deceived about COVID-19, but not about the reasons for their poverty. Just as the British Raj didn’t invest in clean water for its Indian farmers, the U.S. has done little for the health and well-being of its white workers and still less for its Black and Latino workers. And that little has come from the top down, without much consultation. The poor and non-white can be stigmatized for their poverty, and stigmatized again as dirty and dangerous because they’re sick.
“There’s a double paradox here,” de Waal writes of such inequalities. “First, the very basis of the success of our society and economy are what make us susceptible to pandemic influenza, and if we are candid, it cannot be stopped, only mitigated. Second, public institutions must do something, even if it isn’t likely to work, because that’s what they do, and what people expect them to do. Or to put it another way: where science fails, the ‘war on disease’ script fills in the blanks to assure us that science just hasn’t succeeded quite yet.”
De Waal makes a convincing case that modern state power and public health have grown in step since the days of Robert Koch. But public health has always been the state’s political handmaid, doing what it’s told. The state may pretend to follow the science, but only when that suits its political interest.
If public health said pandemics could be stopped only by economic and political equality, its funding would evaporate. The entire business model of the imperial state requires a vast, insecure white working class (made even more insecure by the presence of competing workers of colour). Only insecurity will drive them into low-paid “essential” work, even amid a pandemic, working in meat-packing plants and supermarkets to feed those who make far more money working from the safety of their homes.
That business model also requires the endless invasion of wilderness, turning Amazon forests into cattle pasture and the bats of West Africa into bushmeat, while industrial farming crowds pigs and chickens into ideal conditions for the emergence of new viruses. And of course industry must grow, so its emissions grow, and global heating only adds to the stress and sickness of the poor.
“I suggest that the ecology of the Anthropocene and the social and economic organization of our human population are intrinsically pathogenic,” de Waal says. The imperial states of the past two centuries have exploited their own workers and those in their colonies, with wealth accumulating in each state’s upper classes (and in the state itself). Classism and racism are built right into the state, ensuring unequal social conditions that promote disease as Virchow said. Those conditions have been in place so long that they seem like the natural order of things.
But Koch’s identification of the cholera bacillus as the sole villain enabled Germany and other states to ignore inequality and thereby maintain structural racism and classism. De Waal compares it to our age: “In the same way that the ‘war on terror’ led to a futile effort to end the threat to America by killing supposed terrorists one by one while neglecting the sociopolitical milieu that produced them, so too the new ‘war on disease’ isolated the microbe and ignored the terrain.”
Alex de Waal’s extraordinary book deserves to be read, debated and acted upon. He refuses to offer a solution, just a new word: “pandemy.” Pandemic is just a noun and adjective for the disease. Pandemy is the state of the diseased society. “In using the word ‘pandemy,’ we can reclaim the concept of a holistic disruption, reaching backwards into the ecological, social and health pathologies.... The pandemic needs biomedicine and NPIs [non-pharmaceutical interventions]; the pandemy needs much more.”
Alex de Waal concludes with a modest suggestion: “Emancipatory public health begins with a conversation on this whole-of-society, whole planet, ‘One Health,’ democratic, and participatory agenda. The starting point is not the content of the policies but the process for getting to them. Those who are most vulnerable and most excluded will have some of the most important things to say. This means dismantling the ‘war on disease’ mindset and its politics, assembled over the last two centuries. If we do this, COVID-19 may yet be the emancipatory catastrophe that we need.” ![]()
Read more: Health, Politics, Coronavirus

















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: