Disappointed. Disheartened. Discouraged. That’s how researchers The Tyee spoke with feel about British Columbia’s third wave. They warned the province about the threat posed by coronavirus variants, but the government didn’t listen or acted too slowly.
After successfully battling the first wave and coming closest to mirroring Atlantic Canada’s success story with COVID-19, B.C. has fallen from grace. Besieged by variants and now breaking record case counts, B.C. has joined the ranks of some of Canada’s worst performing provinces. Why?
To get answers The Tyee talked to four prominent experts, including Caroline Colijn, a professor and research chair in mathematics for evolution, infection and public health at Simon Fraser University; Sarah Otto, a specialist in evolutionary biology at the University of British Columbia; Jens von Bergmann, owner of MountainMath, an analytics company; and Amir Attaran, a professor of public health and law at the University of Ottawa.
They attribute B.C.’s missteps to a blend of wishful thinking, poor data, shying from hard decisions and ignoring independent models and reports that correctly foretold the variant crisis.
“I think a lot of people are frustrated,” noted SFU’s Colijn, who warned the province in early February that the variants could explode in March with devastating consequences.
“We had an opportunity to stop the variants, but we didn’t take it,” concurs UBC’s Otto. “We could have gone for zero variants back in January.”
Otto wrote a letter to provincial health officer Dr. Bonnie Henry and the BC Centre for Disease Control on Dec. 22 warning about the highly infectious nature of the new variants, including U.K.’s B117.
That variant killed 50,000 people in just three months, forcing a tight lockdown in the U.K. In particular, Otto warned about “high growth rate in location after location in Europe” that could spell big trouble in B.C. and the rest of Canada.
A month later, Otto again warned that U.K. variant B117 would dominate all cases in a few months. If the province didn’t act immediately to restrict travel, speed up vaccinations and ramp up surveillance, this mutated virus would usher in a third wave.
To better prepare for the variants, the province developed screens that they started using in late January to test samples with a special marker that indicated the presence of one of three types of variants. On Feb. 12, Henry reported that just three variants had appeared in 3,000 samples and that B.C. didn’t have a problem. “If we can just get through these next few weeks,” she said, “I think we’ll be in a much better place.”
But the officially announced results were off by a factor of 10 because the province failed to report the full number of variants it had actually detected.
Nor did the province share the percentage of cases caused by variants, a figure now thought to be about 50 per cent. “It is very challenging for us to make models or predictions without that percentage data,” said Otto.
“I don’t know what the hesitancy was,” she added. “What it meant was that in a critical time in January and February the public did not know what risk they were being exposed to and that allowed a much broader spread.”
The province also didn’t communicate accurately how variants behave. Authorities gave the impression that the variants were replacing the original strain and then stalling. “That is not how things work,” said Otto. “The variants grow exponentially, and they will not stop at 500 cases.”
The evolutionary biologist now warns that the province will “be battling a peak by the end of April and May with peak hospitalizations and ICUs.”

According to Otto, the best thing the province can now do — in addition to tighter restrictions — is to quickly vaccinate the most active and susceptible part of our population: essential workers. She offered two potential COVID-19 futures:
In the best case, the province manages to vaccinate all essential workers by the end of May and “we might be out of the pandemic by the end of the summer.”
In the worst case, the spread of variants outstrips the ability of vaccines to slow infections and mutations. In that case, she said, “We set up an evolutionary race that will keep on scaling up variants that will escape our immune system.”
SFU epidemic modeller Colijn attributes B.C.’s missteps to sparse data, loose borders and poor thinking around the best way to minimize harms. “Allowing another pandemic to take over just a year after the first one is frustrating,” she said.
Colijn offers a metaphor for B.C.’s predicament: a pest control officer who visits a house overrun by mice.
But instead of paying to trap all the mice and to seal off the house, the owners choose to have only half the mice removed, thinking that this will give them half of the benefits. But fast breeding mice soon litter the place with turds, and the house is back to square one.
“This is what we are doing. It’s been Canada’s approach, and one broadly taken up in western countries. And we always wonder why we end up in the same place.” Half measures, she adds, do not give you half the benefits, because COVID is infectious — like mice, it grows back quickly.
At the end of December, Colijn and nearly 20 colleagues recommended a change in COVID-19 response strategy to one named the Canadian Shield.
It said Canada’s six most populous provinces should abandon their rollercoaster strategy, called mitigation, that responds to rises and falls in case numbers by opening or closing some aspects of public life. (Or, as has usually been the case in B.C., trying to do so by pleading with the public to follow shifting rules.)
Instead of that see-saw strategy, the Canadian Shield approach prescribed one rigorous lockdown, firm border controls and ramped up testing for as long as necessary in order to drive infection rates to near zero. The proposal included offering essential workers and hard-hit businesses financial support as the economy took a temporary hit.
The paper got some traction in the Canadian media but little among the public health status quo, although the Canadian government did belatedly strengthen border controls.
But by then the variants had already arrived and were starting spot fires.
On Feb. 9, Colijn published modelling that roughly estimated that the variants would explode the following month. She warned at the time: “The punch line is that failure to prevent or contain this now spells disaster in March.”
In B.C. the warning largely went unheeded. “I think there was a lot of wishful thinking,” said Colijn.

Realizing the speed in which variants spread and the slowness of the vaccination campaign, Colijn and colleagues also urged re-evaluating the emphasis on vaccinating by age groups. Wouldn’t it make more sense to vaccinate the most susceptible and high-risk population that daily encounter lots of people such as essential workers?
Her vaccine model showed that such a strategy in a population of five million people would prevent 200,000 infections, prevent 600 deaths and save nearly a half billion dollars in economic losses.
“You can end up protecting more people per vaccine dose by vaccinating people at risk of exposure and transmission, because it stops the chain before they take off,” explained Colijn.
To Colijn’s relief, the B.C. government indicated last week that it may redirect its vaccine campaign to 300,000 essential workers.
Jens von Bergmann, an independent modeller whose firm has contracted with business, educators and policymakers, believes the province has undermined its efforts with spotty and untimely data, inconsistent messages, and failure to experiment with rapid testing.
In December, he bluntly criticized the province’s many gaps in data reporting in The Tyee. While the province solved some of data deficits, new data gaps emerged as the variants gained strength in the province.
“Basically, on the variants for the last three months we had no data,” said von Bergmann. “And that became a huge issue. Many researchers knew it was going to blow up.” As far back as December, when the variants began to emerge, the need was clear for a system to track variants in B.C., he said. “It took until February to set it up. It was disappointing.”
And, as mentioned higher in this piece, the province’s first snapshot of variant prevalence underestimated the reality. “Only several weeks later did the community learn that the actual counts were 10 times higher, and this was consistently and repeatedly underreported by officials,” said von Bergmann.
“That lead to complacency, and I am still bitter about this because I think it robbed us of our last opportunity to stop variant spread.” Meanwhile, variants started popping up in Fraser Health, the only district that reported variants in schools.
Von Bergmann said the threat posed by the variants was masked by other statistical trends. “While the original strain declined exponentially, the variants grew exponentially. To the authorities it looked like the curve was bending down. In reality, a whole new curve was beginning and started to explode in early March.”
Von Bergmann concludes that some politicians don’t understand exponential growth: the way the steady, repeated doubling of numbers within short times spans can create steep, explosively rising curves.
After the first wave, B.C. drove its numbers down to around 20 cases a day. But in the summer the numbers started to grow, and von Bergmann got worried because “nobody was doing anything. There was always an excuse.” The province didn’t address that exponential growth until November at the height of the second wave.
Von Bergmann became so frustrated, he made an illustration with stick figures that has been widely shared on social media.
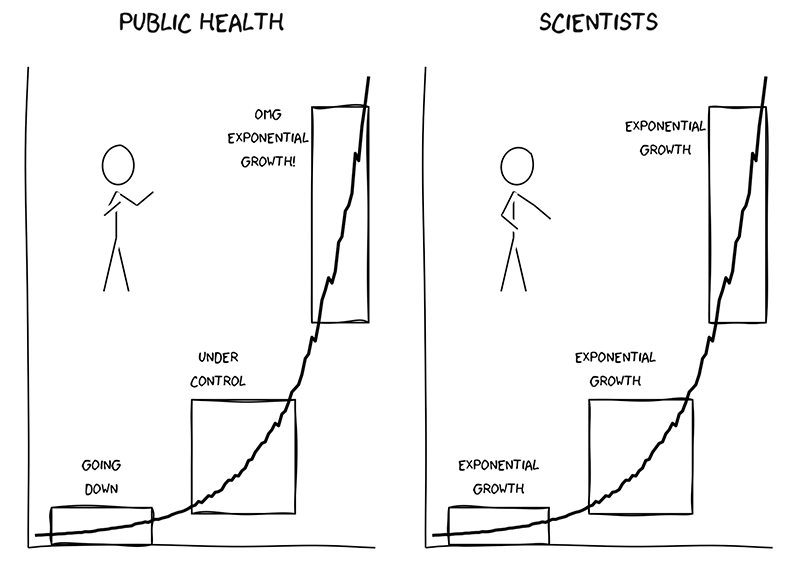
The modeller believes that Premier John Horgan showed his lack of understanding of the exponential dynamic when last week he singled out social young people for causing the rising wave in cases.
“Oh, it must be due to young people partying. But’s that not what’s happening. The variants are accounting for a larger share of the cases.”
Von Bergmann suspects that the so-called “three-week circuit breaker” that Henry and Health Minister Adrian Dix introduced last week will likely last to May because the variants are harder and costlier to fight. And it will take that long to vaccinate the population. He remains uncertain the current restrictions will do the job. It is unlikely the variants can be contained without stay-at-home orders, he said.
Von Bergmann sees more concerns ahead and hopes they’re on the radars of B.C. health officials. “Probably sometime this summer we will be dealing with escape variants that elude the vaccines. I doubt this will be over by fall. We will be in this fight for quite some time as far as I can see.”
For University of Ottawa professor of public health and law Amir Attaran, the bad place B.C. has landed is confusingly “out of character.”
As a French study pointed out last week, Canada’s six largest provinces, including B.C., have failed to achieve the success modelled by the nation’s smaller provinces and territories, which took a more aggressive “COVID zero” approach of the kind proposed by the Canadian Shield report.
Still, with some of its practices early on in the pandemic, B.C. “seemingly attempted to pursue a COVID zero policy” more than the other large provinces. “And now they have clearly repudiated it,” said Attaran.

Attaran sees a key turning point in Horgan’s abrupt election call last October.
At the time Horgan, then accountable to a minority government, claimed that he needed a new mandate from the public in order to form a majority government to address the full weight of the COVID-19 crisis. Only a majority government could create “more security for everyone in British Columbia,” and shield its residents from the next pandemic, argued Horgan’s election platform.
“COVID-19 has shown us what can happen when an unexpected and overwhelming health crisis occurs. Our job is to make B.C. ready for the next one.”
The next pandemic, however, in a sense arrived in January, as the virus mutated into variants. What’s happening in B.C. now can be regarded either as the first wave of a new pandemic driven by Brazilian and U.K. variants, or simply the reignition of the second wave, which the province never got under control, argued Attaran.
But Horgan and his NDP government haven’t used their voter mandate to make potentially politically unpopular choices needed to fight the rise of the variants and keep people safer, he said. That would have included masks in schools, tighter border controls, rapid testing and lockdowns when the variants arrived.
Instead, exponential growth of the variants is now rapidly unnerving the province and is poised to put more young people in hospital with serious illness.
“Horgan was much more solicitous to public health and protecting people before the election than after,” concluded Attaran.
Von Bergmann said the province and the country have been let down by leaders who never conducted the public conversation needed to educate people about competing ideas of how to battle the virus, and weigh the possible risks and rewards.
“The biggest decision is, do you want a mitigation policy or COVID zero or near elimination strategy? We have never had a discussion about these choices. No one in Canada (except Atlantic Canada) has had that. And that’s a systemic failure.”
SFU professor Colijn, whose specialty is using mathematical modelling to peer into the potential futures of epidemics, shakes her head knowing that, months ago, the data on the B117 variant from England clearly illustrated how it would accelerate the pandemic.
“Yet until we saw the same pattern in our local data, we didn’t act. We didn’t need to wait, but we did. And that’s not just a Horgan problem, but a Canadian one.” ![]()
Read more: Coronavirus

















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: