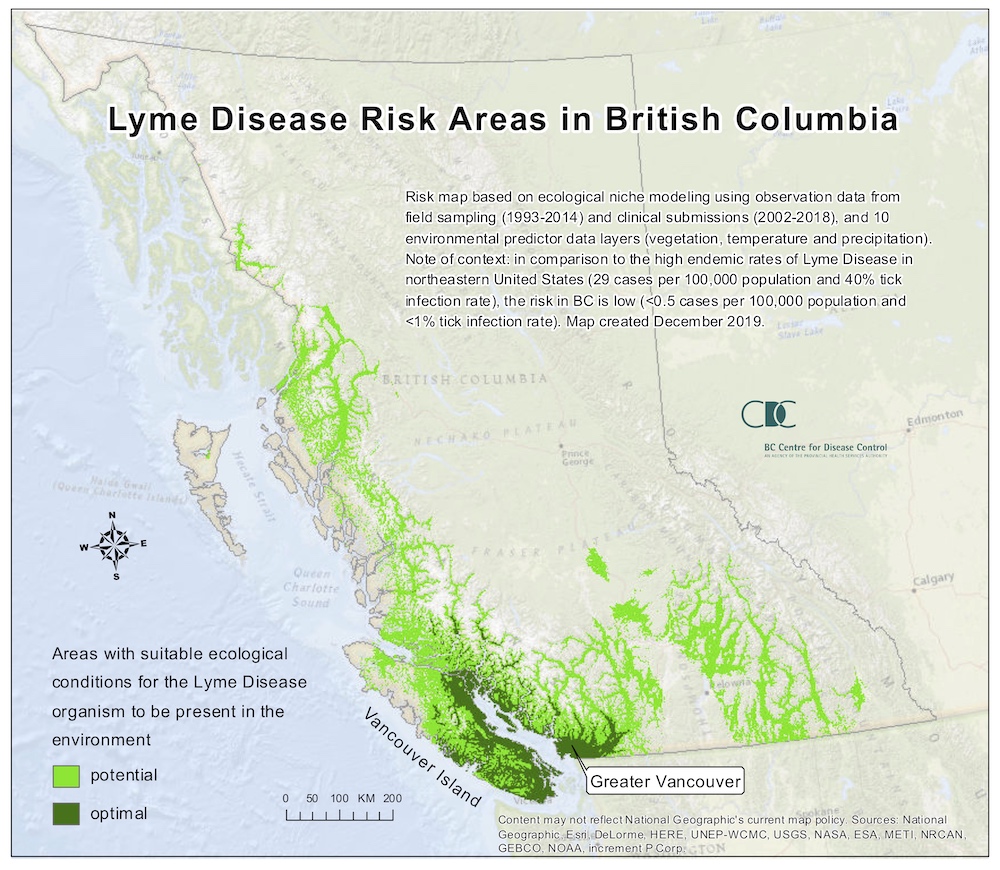
On the BC Centre for Disease Control’s website, a map shows where Lyme disease exists in the province. It highlights isolated areas in the south, mostly focused around Vancouver Island and the Lower Mainland, extending as far north as Clearwater. In the north, there are pockets of “potential” around Williams Lake and in coastal areas.*
But the map, dated 2019, leaves vast swaths unmarked and the impression that Lyme disease is not a risk from tick bites in most of the province.** As a result, it can be hard to get your doctor to listen if you have Lyme symptoms and even harder to get a conclusive diagnosis.
Officially, Lyme, spread by bites from infected ticks, has only been positively diagnosed a handful of times in the northern three-quarters of the province.*** But some experts say that’s because its myriad symptoms — everything from joint pain to facial paralysis — are often misdiagnosed as illnesses like chronic fatigue, fibromyalgia, multiple sclerosis and early dementia.
And its official absence may be perpetuating a myth by making it hard to get a diagnosis or testing.
“If you get robins in the spring, if you get migrating birds, then you have potential for Lyme disease,” says Canadian Lyme Disease Foundation president Jim Wilson. “There is no part of B.C. that is Lyme-disease free.”
A decade ago, when Bridie O’Brien found a tick on her Pomeranian-Chihuahua cross after it had been roaming the bush north of their Hazelton home, she pushed her vet to send the specimen away for testing. When the results finally came back, O’Brien learned that the tick that had bitten her dog — who would go on to suffer Lyme-like symptoms — carried the Lyme-causing bacteria Borrelia burgdorferi.
“The vet told me they tested it three times because they were so sure it would be negative,” she remembers.
Testing for Lyme is not an exact science. In B.C., it starts with a screening test called ELISA that looks for antibodies in the blood. The results are interpreted based on factors such as seeing the tick bite, where the patient lives and whether they’ve travelled. The fact that Lyme is considered non-existent in much of the province affects those assessments.
Even if the test shows the antibodies, “an in-house assessment is made on whether it’s a false positive,” Wilson says.
If the initial test is deemed positive, a second test, the Western Blot, is used to confirm the diagnosis.
If the number of Lyme markers detected suggests a borderline diagnosis and you live somewhere considered low-risk, your geographical location could be the determining factor in the diagnosis.
Jennifer Atkins, a former Smithers resident, was tested for Lyme after several years of symptoms like numbness, fatigue, dizziness and visual disturbances. The test came back negative. After investigating for multiple sclerosis, Atkins visited a naturopathic doctor in Vancouver for a second opinion.
“I still wasn’t convinced these symptoms weren’t Lyme related,” she says. “I had a second — different — test run in July, which came back positive.”
The second test was ordered through IGeneX, a private lab in California. Going out of country for both testing and treatment is a route many Canadians are taking.
But Muhammad Morshed, a clinical microbiologist with the BCCDC, says private labs are notorious for inaccurate results, with false positives reported up to 50 per cent of the time.
For Atkins, it’s a relief to have answers. After four months of antibiotics, her symptoms significantly improved. But her positive diagnosis, like others done outside the country, are not included in the 18 official cases diagnosed in B.C. in 2018.
Wilson accuses the province of artificially suppressing Lyme numbers, calling the BCCDC’s estimated tick infection rate of less than one per cent “absurd.” According to Wilson, the infection rate is closer to four per cent province-wide and up to 40 per cent in some areas.
Entomologist Janet Sperling notes that Borrelia burgdorferi strains vary geographically, with research indicating that Lyme tests become less effective the farther west you go. While her PhD research at the University of Alberta examines ticks collected by tree planters across B.C., results won’t be available for several years.
“There are areas that are more likely, such as the Sunshine Coast, Vancouver Island and Greater Vancouver,” she says. “We know that the problem certainly goes as far as Williams Lake. How much farther north? I don’t know because nobody’s really been looking.”
Morshed admits that his research has only once taken him into northern B.C. “The problem is that active surveillance is costly and nobody wants to give money for surveillance studies,” he says. Instead, the BCCDC funds passive surveillance, which invites the public to send ticks they find for testing.
Since most Borrelia burgdorferi is carried by nymph ticks, which are smaller than the head of a pin, the adult ticks that are most often submitted for testing are far less likely to carry the disease.
Morshed stands by the BCCDC’s map.
“I think the map is still valid and will provide an overall idea about risk, but not true incidences,” he says. But people should not be discouraged from investigating possible Lyme cases, he adds. “Lyme disease bacteria exist in B.C., and I have proven that over and over and over.”
Staying vigilant about the disease — particularly after getting a tick bite or seeing erythema migrans, the bull’s-eye rash indicative of Lyme — is especially important when its early detection can mean the difference between a course of antibiotics or living with debilitating chronic illness.
“Based on everything we know, the risk is lower in northern B.C.,” Sperling says. “But that doesn’t mean it doesn’t exist.”
*Story updated Sept. 1 at 4:15 p.m. to correct the areas on the BC Centre for Disease Control’s map where there is a potential that Lyme disease exists.
**Story updated Sept. 1 at 4:15 p.m. to correct the date of the BC Centre for Disease Control’s map of Lyme disease. It is dated 2019, not 2013.
***Story updated Sept. 1 at 4:15 p.m. to correct that Lyme disease has officially been positively diagnosed a handful of times in the northern three-quarters of the province. ![]()
Read more: Health, Science + Tech

















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: