Laura Shaver’s phone rings at all hours. It rings when she and her partner are dealing with mould in their apartment, interrupting texts to their landlord. Calls from Ontario come in at six in the morning, where it’s already an acceptable time to do business but Shaver is still asleep.
She’s just one person, but it’s Shaver’s job to answer the phone. As Providence Health’s peer navigator for opioid agonist therapy, or OAT, she’s the point person for people who use drugs and are seeking access to substitutes for opioids, a first-line treatment in British Columbia where the street drug supply has grown increasingly toxic.
The callers are mostly trying to access opioid agonists like methadone or Suboxone, which play on the same receptors as opioids themselves and prevent withdrawal sickness without the same feeling of a high. Other times, they’re trying to reach a prescribed supply of benzodiazepines, which doesn’t exist in the province.
All day long, Shaver fields callers who want to reduce their reliance on toxic street drugs. She guides them through an inaccessible patchwork of treatment options that wasn’t built to handle their needs. It’s not just that callers can’t get the amount of drugs they want or that they can’t access a specific type of treatment, she said. “It’s that they can’t get treatment at all.”
Even as the poisoned drug crisis worsens, medical therapies to remove people from the street supply, like opioid agonist treatments, remain financially and geographically inaccessible to the vast majority of B.C.’s more than 88,000 opioid-dependent people.
About 23,000, or less than one-third of the group, currently take some form of OAT, according to B.C.’s most recent count provided to The Tyee.

Despite the clear gaps in treatment, the B.C. government says the pandemic has put a hold on work to fund, support or regulate the private clinics that are mostly diagnosing, prescribing and supporting people who use drugs.
Thousands more people who wish to access treatment remain without a physician who will prescribe to them, a private opioid agonist clinic close enough to them, or the money to pay the clinic fees or for the prescriptions themselves.
“I lose people weekly, daily, because our government refuses to prescribe the things people need,” said Shaver, who’s also a board member of the Vancouver Area Network of Drug Users. About six people are dying of toxic drugs each day in B.C. in 2021.
Patients, advocates and health-care workers say the lack of standards and continuity forces people who use drugs to pay for lifesaving care the public system doesn’t have capacity to provide.
“When there is an inquiry into the overdose crisis, they’re going to find out the practices of the entire methadone system are at fault,” said Garth Mullins, a board member of the BC Association of People on Opioid Maintenance who’s used methadone for nearly two decades.
A lifeline for drug users
The last 25 years have seen opioid dependence increase rapidly, bringing new urgency to the need for accessible treatment. But opioid agonists are not new in Canada.
Vancouver is home to North America’s (and likely the world’s) first use of methadone for opioid maintenance, a program Dr. Robert Halliday started in 1963. His research findings went on to form the evidence base for establishing opioid agonist therapy across Canada.
OAT typically involves an individual visiting a pharmacy one to three times per day for observed dosing by a pharmacist. Once someone is considered stable, they can begin taking “carries” home — up to a three days’ supply of their medication.
When prescribed at an effective dose and coupled with housing and social supports, OAT can be instrumental for people with substance use disorder who wish to reduce or stop accessing the street drug supply altogether.
(This is not the same as safe supply, which aims to save lives by separating people from the toxic street supply by prescribing regulated doses of pharmaceutical-grade substances like heroin itself.)
Since the College of Surgeons and Physicians changed its guidance for physicians in 2017, methadone, Suboxone and other opioid agonist therapies can be prescribed by any physician in B.C. who follows training from the regulatory college, as well as a growing number of nurses under a 2020 public health order.
The change brought a number of new and private addictions medicine clinics into the system. Willing doctors from other practice areas like family medicine and psychiatry now focus some of their work hours on diagnosing patients and prescribing alternatives.
But many doctors remain unwilling or hesitant to prescribe opioid agonist therapy, citing concerns about liability for potential overdose or patients reselling prescriptions to others. (According to the BC Coroners Service, neither methadone nor Suboxone has ever been found to have contributed to a fatal overdose since monitoring began in 2016.)
The capacity these private clinics offer can be a lifeline — and the only option — for people like Shaun Venturini who want to seek treatment for their substance use disorder when public clinics are full.
Pacific Oak, a private clinic in Vancouver’s Downtown Eastside neighbourhood, became like a “second home” for Venturini when he sought treatment last November.
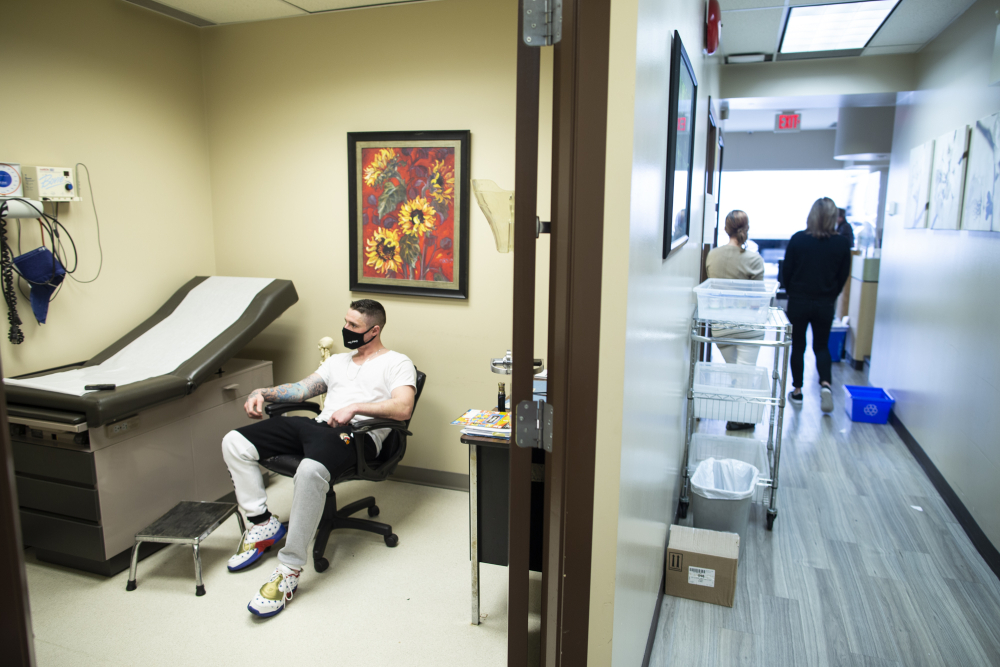
He started using heroin and methamphetamines when he was 25, shortly after his then-girlfriend introduced him to the prescription opioid OxyContin. In the last eight years he estimates he’s overdosed more than 30 times and has been arrested multiple times for survival crimes to afford his next dose.
Venturini decided many times before last fall that he wanted to stop, but had trouble finding a spot in a detox facility, which can provide the necessary support for people transitioning from using onto opioid maintenance. Pacific Oak helped him find a spot in detox in November and started him on methadone soon after.
Now 33, Venturini says his desire to use opioids is mostly gone. He has stable social housing and plays hockey, his childhood sport, with the clinic manager Fiona Knight’s grown daughter, Sophie.
“I’m working on a book about my life. I feel like a kid again,” he told The Tyee.
Patients footing the bill
Private OAT clinics provide an essential service by bringing together doctors willing to prescribe under one roof, so patients can easily find them. Of the nearly 300 patients Dr. Jay Wortman sees at Pacific Oak’s sister clinic Royal Oak in Vancouver, two have died of overdoses in the last two years.
“Those are remarkably low numbers. It strikes me... it’s not the fact we’re handing out methadone, it’s that we’re treating them with respect and compassion,” said Wortman.
But unlike public OAT clinics, which are concentrated in the Downtown Eastside, private clinics don’t receive public funding for rent or materials. Doctors still bill the province through the regular fee-for-service model, but nothing else is covered.
The fee-based model incentivizes limited staffing and fluctuating scheduling structures, which makes the treatment experience unpredictable.
“People that are on any type of opiate, they need to have routine,” said Shaver.
Many clinics have limited hours based on physician availability and are only able to give hours-long windows in which people arrive to join the queue to be seen.
You never know which doctor you might get, Shaver said, and having to re-explain your life or preferences can impact the strength of relationships and the quality of care.
Most people don’t have the transportation or time to go to a doctor even once a month to keep up their prescription, said Shaver.
If you miss an appointment your prescription can be cancelled, and the process starts all over again. “Private clinics can make their own hours and people have no choice but to go and wait outside to make sure you’re there first, because they need a script and a doctor,” said Shaver.
To stay afloat, the clinics also charge monthly fees of around $60 per patient. Pharmacists also charge clinics prescription and dispensing fees, which can be as much as $14 per day.
The province pays these fees and the vast majority of prescription costs for about 7,700 people on income or disability assistance. But that leaves more than 15,000 patients, many working poor and low-income, who have to pay their own way.
Patients who aren’t considered poor enough to have their prescriptions covered by the province have to pay nearly $500 per month — $6,000 per year — for treatment the public system doesn’t have the capacity to adequately provide.
The cost can be an added barrier for people who wish to seek employment once in recovery but fear losing their treatment coverage if they earn more.
“It is better than nothing, and it’s a huge impediment, because half the people on methadone, they’re not on welfare, they have to pay for it. A lot of people aren’t going because of those fees,” said Mullins.
A spokesperson from the Ministry of Mental Health and Addictions said in an email that while the province is aware that fees can be a barrier for people who don’t qualify for coverage, it is not currently considering covering them universally.
“I just wish that everyone was covered. It feels wrong to collect fees,” clinic manager Knight told The Tyee from an examination room at the Royal Oak clinic on Commercial and Broadway. She also runs the Pacific Oak clinic where Venturini is a patient.
Knight began managing Royal Oak in 2008 and Pacific Oak a few years later. Her stepfather, Dr. Philip McCormack, was one of the first doctors in B.C. to begin prescribing OAT out of his family practice in Surrey in the late 1990s, and Knight recalls his practice evicted him for doing so.
Later, McCormack moved to an office down the street where he practiced and prescribed methadone until age 82. His determination piqued Knight’s interest in providing much-needed treatment to vulnerable patients.
When doctors from her clinic and others founded Addictions Care Clinics of B.C. in 2018 and began to call for provincial support, regulation and standards, it was largely to rein in “bad apple clinics,” Knight said.
In 2018, she visited Victoria with colleagues to advocate for further integration into the public system and felt it went well. But since the pandemic, it’s been silence from the government, Knight said.
“We can be a part of the solution. We are part of the solution already, but we aren’t recognized at all.”
Restrictions on prescriptions
Today’s prescribing guidance for OAT often fails to recognize that many who seek treatment still use criminalized substances from the street supply on the side, increasing the risk of overdose.
If someone discloses they are still accessing the street supply, prescribing guidance says they can only begin building up OAT dosages again once they are substance-free.
The buildup of dosages can take more than a week with multiple doctor visits, during which people are going through withdrawal with a lowered tolerance. This period is when their risk of overdose is highest.
The distances and stringent appointment and monitoring requirements also make it hard for those who work long hours or have unreliable transportation to stay on their treatment plan.
Before Reija Jean moved to the Downtown Eastside, where she had access to an integrated public clinic for residents only, she was taking the SkyTrain from Vancouver to New Westminster every week on her day off to visit the clinic to assess her dosage. It was a costly and time-consuming journey that many can’t easily make.
“You’re there all day. I was lucky I had the day off,” said Jean, who’s been on OAT since 2017.
Urine testing is also used to determine whether someone has been using drugs, which further dehumanizes patients during this process, though the practice is not unique to private clinics. Getting a positive result potentially means no longer getting “carries” — up to three days’ supply to take home — or worse, being cut off.
With all the barriers people face to access OAT, many turn to drugs that are more readily available on the street when their doses get cut. By limiting a safer alternative, prescribers often drive people to use more, Shaver said.

Dr. Edith Moser, who’s prescribed methadone in B.C. since 1998, describes her 70 or so patients at Royal Oak and a Surrey clinic as a relatively stable group, which used to be the norm before the street drug supply became so poisoned.
Restrictive guidance that limits how quickly doctors can measure out doses for patients who’ve used street drugs remains a real barrier to starting people on methadone and making it a real alternative to the criminalized street supply.
To have people forced to pay for it when the risk of overdose is so high is “blatantly discriminatory,” Moser said from her exam room at Royal Oak.
BC’s program no longer world-class
The current government has time and time again touted its expansion of treatment options like OAT as a significant measure, while six people continue to die each day and progress on decriminalization and safe supply remains painfully slow.
But one wouldn’t know Vancouver was once a world-leader in opioid maintenance by looking at the province’s “system” today, says Mullins.
Waits at public clinics are long, and very few public clinics are listed through the BC Centre on Substance Use’s most recent OAT clinic list.
The province has said it is working on expanding rapid access clinics in all health authorities, including Fraser Health’s second that opened at Royal Columbian Hospital in New Westminster in February.
And there are some public clinics, like the Downtown Eastside Connections Clinic, that do work with integrated primary care. (A request to interview the director of Connections Clinic or another public OAT clinic was denied by Vancouver Coastal Health.)
But advocates say the government has failed to recognize that the toxic drug and opioid poisoning crises reach all neighbourhoods and people of all incomes and backgrounds.
“Private clinics exist because there is demand for the service outside the Downtown Eastside,” said Jean, who’s working on OAT patient resources with the BC Centre on Substance Use to help patients advocate for themselves. The centre also recently received provincial funding for Shaver to hire more patient navigators.
Despite loosened prescriber eligibility, physician hesitancy has seen OAT remain in the hands of few B.C. doctors. Many patients, particularly in remote communities outside of the Lower Mainland, still have difficulty finding a doctor who will prescribe them anything at all.
B.C.’s health-care system has “essentially carved methadone and OAT in general out of the public system,” said Mullins. He estimates over the last 19 years he’s paid upwards of $11,000 alone for his clinic fees and prescriptions.
And without proper regulations on enforceable standards around hours, patient care or funding, B.C. has left people who use drugs vulnerable when seeking treatment.
“You can really see the government’s lack of commitment to the overdose crisis, not by what they do on the big stuff like decriminalization, but by what they do on the little stuff like OAT,” said Mullins. “There are small reforms which could have some really big payoffs in terms of lives saved.”
As a patient navigator, Shaver helps advocate for people who have been tapered off or denied a prescription, or otherwise turned away from OAT. “It’s wrong, it’s so wrong, and nobody even knows that they have a right to complain about that.”
Patients at public clinics can complain through the Patient Care Quality Offices unique to each health authority, but private clinics fall outside the office’s jurisdiction. For those, issues must go straight to the BC College of Physicians and Surgeons, but it’s an arduous process that’s usually resolved or dropped before it reaches the formal complaint stage, Shaver said.
In the meantime, she continues to leave her phone on “ring.” She fears missing a call where she could have helped connect someone to OAT, someone who may end up using poisoned drugs.
And she is most worried that one day the calls will stop. “There’s only a matter of time until there’s nobody left alive.” ![]()
Read more: Health, BC Politics

















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: