A new drug-user advocacy group in Vancouver says the safe supply of prescription narcotics must include pharmaceutical-grade heroin and cocaine and — to kickstart the effort — they’ve started giving those drugs away for free themselves.
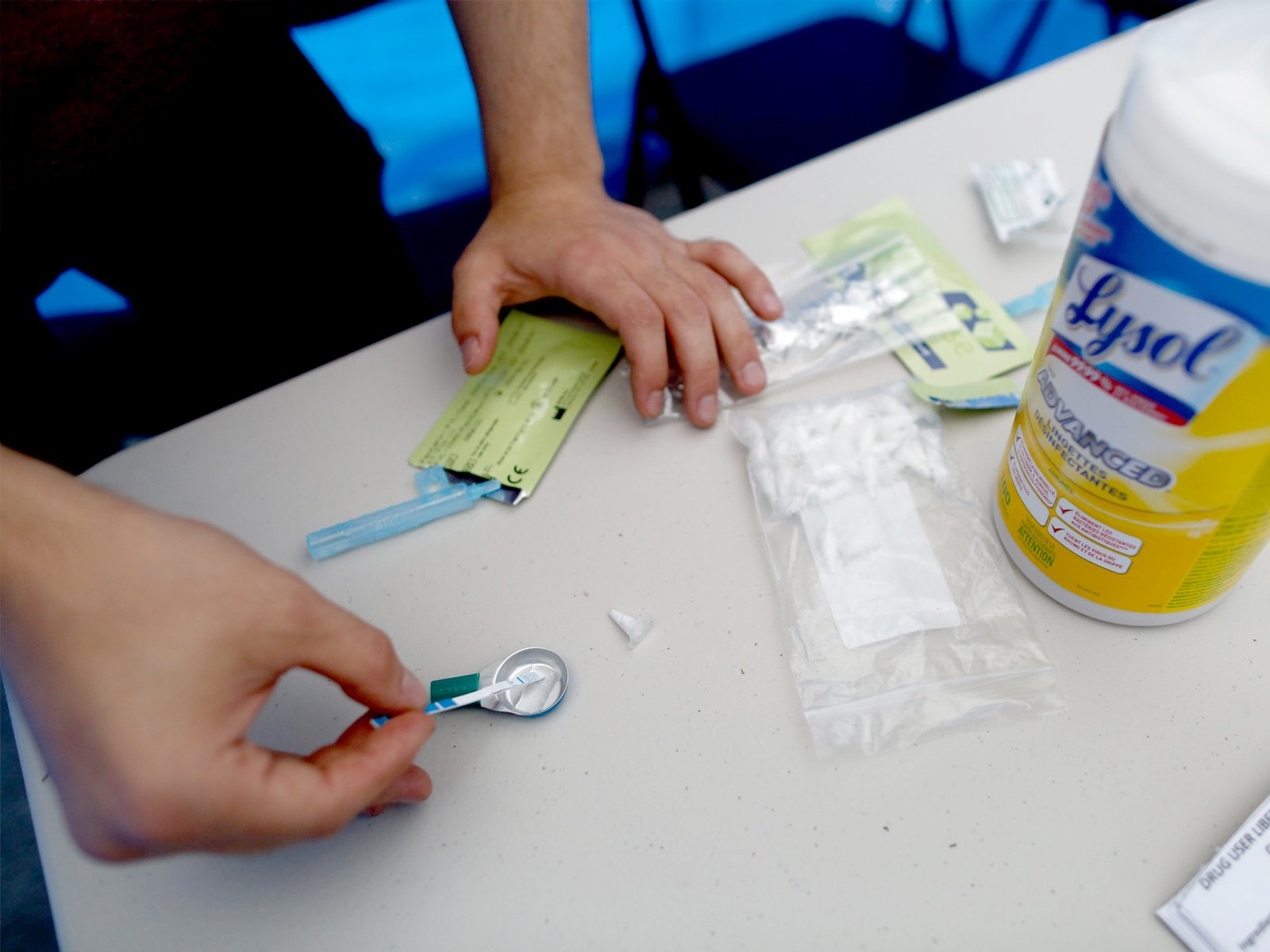
Today, dozens of people who use drugs marched in the city’s Downtown Eastside and set up an overdose prevention site at the corner of East Hastings Street and Dunlevy Avenue, where they distributed free doses of cocaine that had been tested for fentanyl, carfentanyl, benzodiazepines and other dangerous contaminants.
Organizers had planned to distribute up to 200 doses of free heroin as well, but existing supply lines have become so contaminated that they couldn’t find any.
“It really speaks to the level of contamination that’s out there on the street,” said Jeremy Kalicum, one of the demonstration’s organizers.
Calling itself the Drug User Liberation Front, the group also called on the B.C. government to make broad changes to the current safe supply guidelines. The government should eliminate barriers preventing people from accessing life-saving medication in the midst of the worst spike in overdose deaths since the crisis began at least five years ago, they say.
“I’m at risk of an overdose,” said Hawkfeather Peterson, a user and advocate who says their family doctor refused to prescribe them an opioid alternative because they “doesn’t seem like a drug user.”
Being denied “put my life at immediate risk,” Peterson said. “People have some pretty archaic notions of what substance use looks like.”
The new safe supply prescription guidelines were introduced by the province in late March as an emergency measure during the COVID-19 pandemic. They allow doctors and nurse practitioners to prescribe take-home pharmaceutical alternatives to people at risk of an overdose from an increasingly toxic and dangerous street drug supply.


At 170 deaths, May was the deadliest month on record in B.C.’s ongoing overdose crisis, with most deaths attributed to “extreme” fentanyl concentrations in the drug supply, according to a B.C. Coroners Service report.
Since January 2016, more than 5,545 in people in B.C. have died of an overdose.
According to the Ministry of Mental Health and Addictions, prescriptions for the opioid street-drug alternative hydromorphone increased 149 per cent from 677 to 1,686.
Uptake has varied across each of B.C.’s health regions. The Fraser Health Authority saw the largest increase in prescriptions, up 236 per cent from 101 to 339. Vancouver Coastal Health saw the number increase 216 per cent, from 240 to 759. Island Health was up 144 per cent, Northern Health was up 188 per cent. The Interior Health Authority saw by far the smallest increase at 27 per cent (from 161 to 205).
The safe-supply program, at first hailed as a breakthrough in harm reduction strategies, has since come under fire from drug users and advocates over the barriers many say they face in accessing the program.
Peterson is part of a Vancouver-based heroin compassion club that they say has been running for about a year.
“It basically operates by having a group of safe community members that can help each other source and locate heroin that doesn’t have fentanyl and is tested for it,” they said.
The group members work to share costs and source a reliable quantity of drugs to maintain a steady supply, similar to how cannabis compassion clubs operated in the early days of the push for legalization of that drug, Peterson said.
But even with the help of the compassion club, sourcing clean heroin has become virtually impossible, Peterson said.
Border restrictions and other measures meant to combat the COVID-19 pandemic have thrown an already unstable illicit drug supply into chaos, cutting off access to the raw materials and making the street supply almost entirely contaminated.
Peterson said they and many other members of the compassion club have tried to get access to the safe supply programs but have been denied.
“Almost every single person I know in the compassion club is a mother with children,” Peterson said. “They’re not bad parents. They’re just trying to stay alive and be well... but there is so much stigma around substance use and parenting.”
Peterson said several members of the club who have tried to access narcotic alternatives through their family doctors have not only been refused. Their doctors have threatened to call Child Protection Services on them.
Erica Thomson, the executive director of the BC and Yukon Association of Drug War Survivors said there is growing anecdotal evidence to suggest barriers to existing safe supply are disproportionately faced by women.

Thomson said one of the problems with the existing hydromorphone alternatives is that they are designed to discourage injection use, making them difficult to crush and inject.
Instead of the name brand Dilaudid, some users have also reported being prescribed generic versions of the drug, which contain more chalk and other additives that make them dangerous for injection users.
“It can clog up your needles, which can increase the risks of people sharing needles,” Thomson said, “or you end up injecting chalk into your veins.”
For many users, hydromorphone doesn’t provide the feelings of euphoria or emotional tranquility that they experience with other opioids, especially important for people struggling with emotional trauma.
“Hydromorphone isn’t the same, just like methadone and Suboxone isn’t the same. They’re all very different drugs. Is it an opioid? Yup, but it’s not the same and having control over your medication is important,” Thomson said.
In a statement, the Ministry of Mental Health and Addictions called the challenges faced by people who use drugs “unprecedented.”
“We are working as fast as we can to keep people safe by separating them from the toxic, illegal drug supply,” the statement said.
“We are aware of some of the concerns and are working with our partners to ensure the (prescription) guidance works for everyone. We will continue to evaluate its effectiveness and update as needed,” the statement said.
Dr. Ashley Heaslip is a family physician at an inner-city clinic in Victoria and the medical lead at PHS Community Services Society. She said there are systemic barriers in the safe-supply system that need to be addressed.
“The fact that the program is driven by prescribers is a real challenge,” Dr. Heaslip said.
“If people don’t have access to an initial prescriber who is willing and able to start the prescription and also who is able to work with them consistently throughout the course of whatever that prescription looks like for them, obviously that’s going to be very challenging,” she said.
Heaslip said PHS Community Services Society is lucky to have a level of wraparound support for its clients that not all doctors or other prescribers have.
“We have access to pharmacies who actually deliver medication to individuals and ensure that they’re accessing on a regular basis what we’re prescribing. That’s not a common reality in a lot of rural or even suburban locations,” Heaslip said.
“My understanding is that the guidance is being interpreted and delivered in totally different ways across the province,” she said.


The organizers of the demonstration say they want to see the B.C. College of Physicians and Surgeons issue a statement backing the new prescribing guidelines so doctors know they’ll be supported in following them.
They also want to see simple possession of drugs decriminalized, and the Vancouver Police Department defunded, with money redirected towards community-led overdose response initiatives.
As for the call to add cocaine and prescription heroin, also known as diacetylmorphine, to the options available under the safe supply model, Dr. Heaslip said the overdose death figures make one thing clear.
“When you look at those overdose numbers from May, nobody can turn a blind eye to the impact of that devastation. Every single option that could possibly be on the table I think is on the table right now.”
*Story corrected at June 25 at 2:30 p.m to reflect the correct pronouns of Hawkfeather Peterson. We apologize for the error. ![]()
Read more: Health, Rights + Justice, Coronavirus
















Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion.
*Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
Do:
Do not: